Optimizing patient and staff care: the crucial role of efficient workflow in the operating room and ICU
Did you know that behind every successful surgery and critical patient care lies complex medical equipment and a team of highly skilled professionals? The key lies in sophisticated medical equipment and coordinated collaboration among healthcare professionals.
“These aspects materialize through efficient workflows in the Operating Room (OR) and Intensive Care Unit (ICU), crucial elements ensuring optimal outcomes for both patients and medical staff.”
Crucial Coordination: The Determining Role of Workflow in the OR and ICU
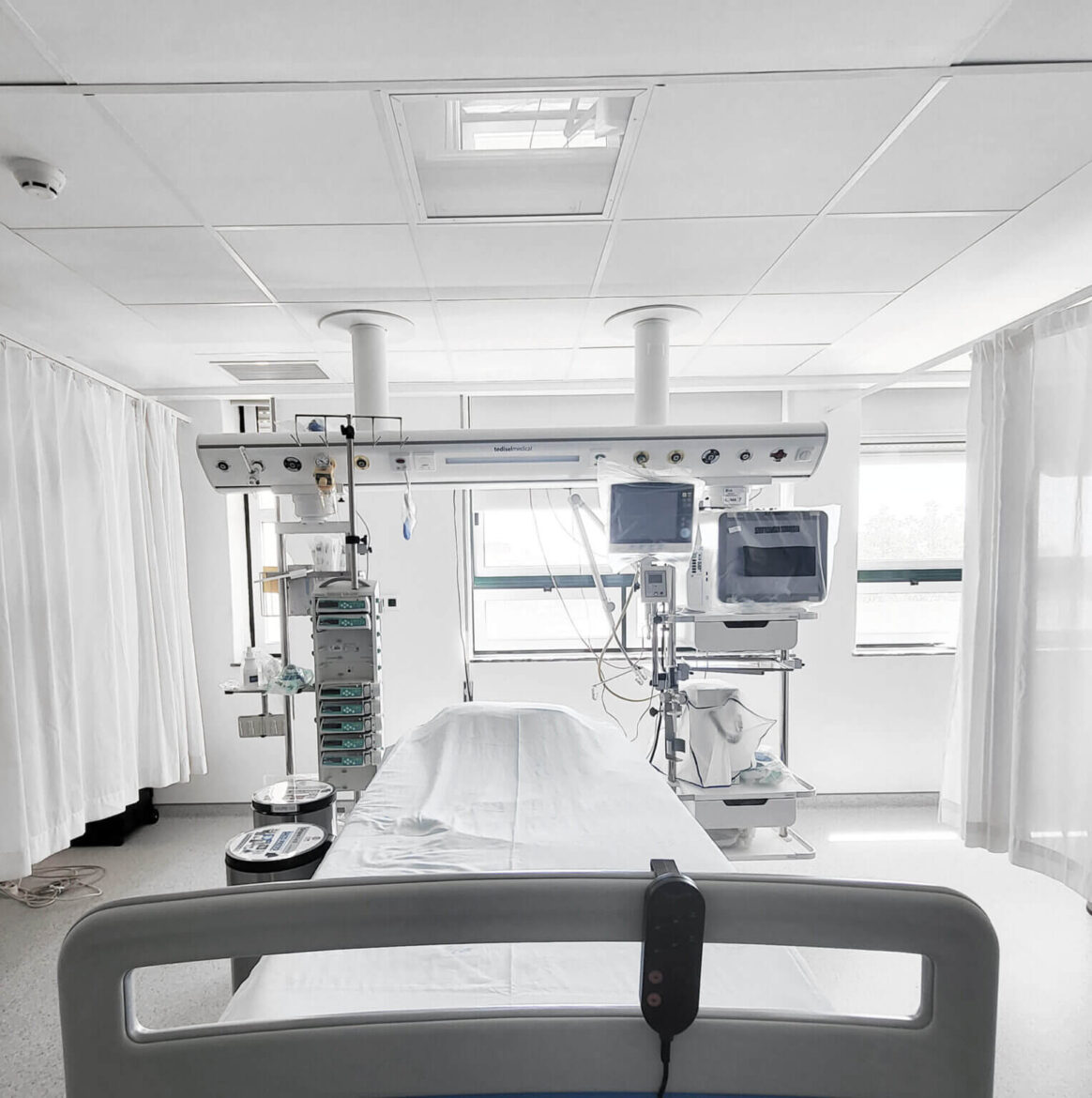
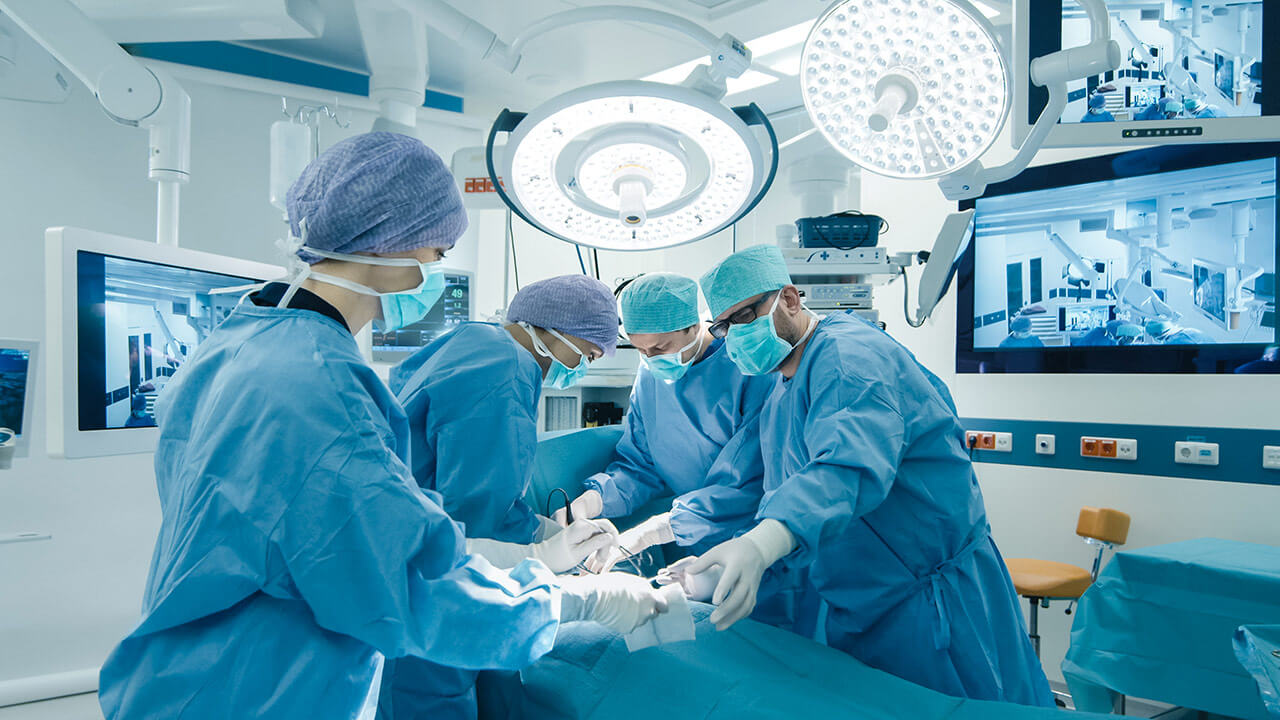
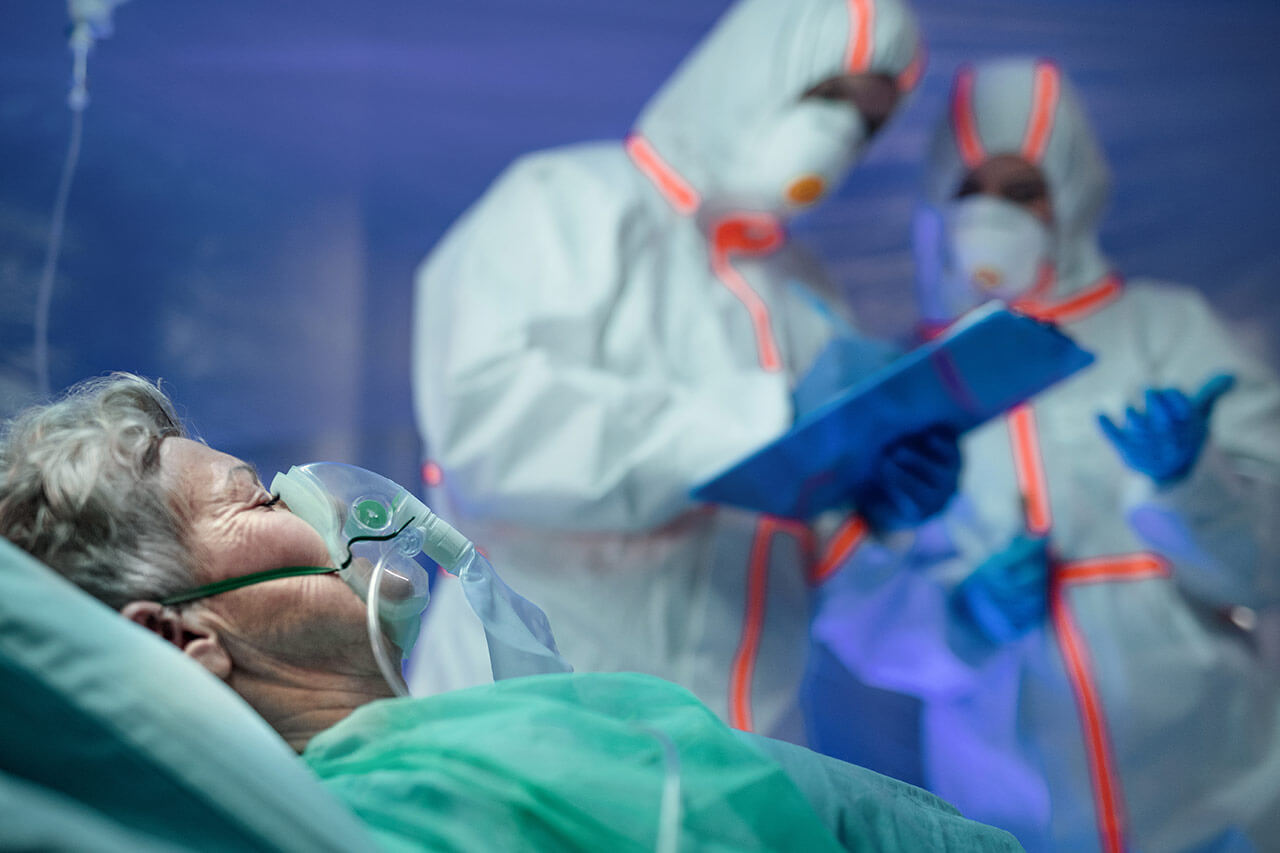
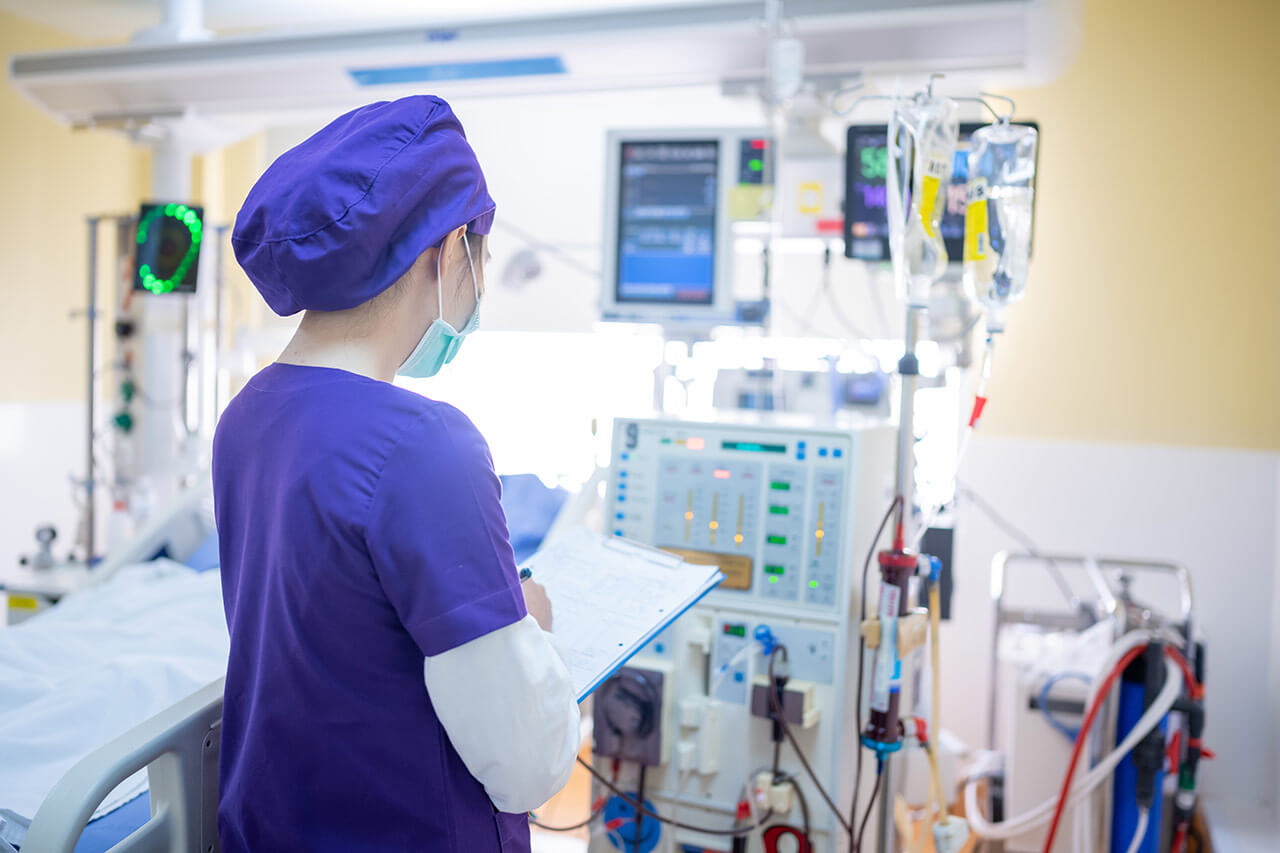
Efficient workflows in the OR and ICU play a crucial role in reducing errors and ensuring seamless coordination among healthcare professionals and hospital staff. In the OR, centralized and well-coordinated optimization involves precise steps such as patient preparation, anesthesia administration, and surgical execution. Collaboration among surgeons, anesthesiologists, nurses, and support staff is imperative to provide the best patient care. Similarly, workflow in the ICU focuses on continuous monitoring and treatment of critically ill patients, requiring effective communication and coordination to address changing patient needs.
Effective workflow management goes beyond mere efficiency; it constitutes a critical component in both patient and clinical staff experience, encompassing aspects of safety and positive health outcomes. Given the gravity of the consequences that can arise from errors or delays, hospitals must make significant investments in high-quality medical equipment to minimize potential risks. In this context, the contribution of Tediselmedical stands out, offering a wide range of models specifically designed for the ICU and OR, providing optimal solutions for hospital environments.
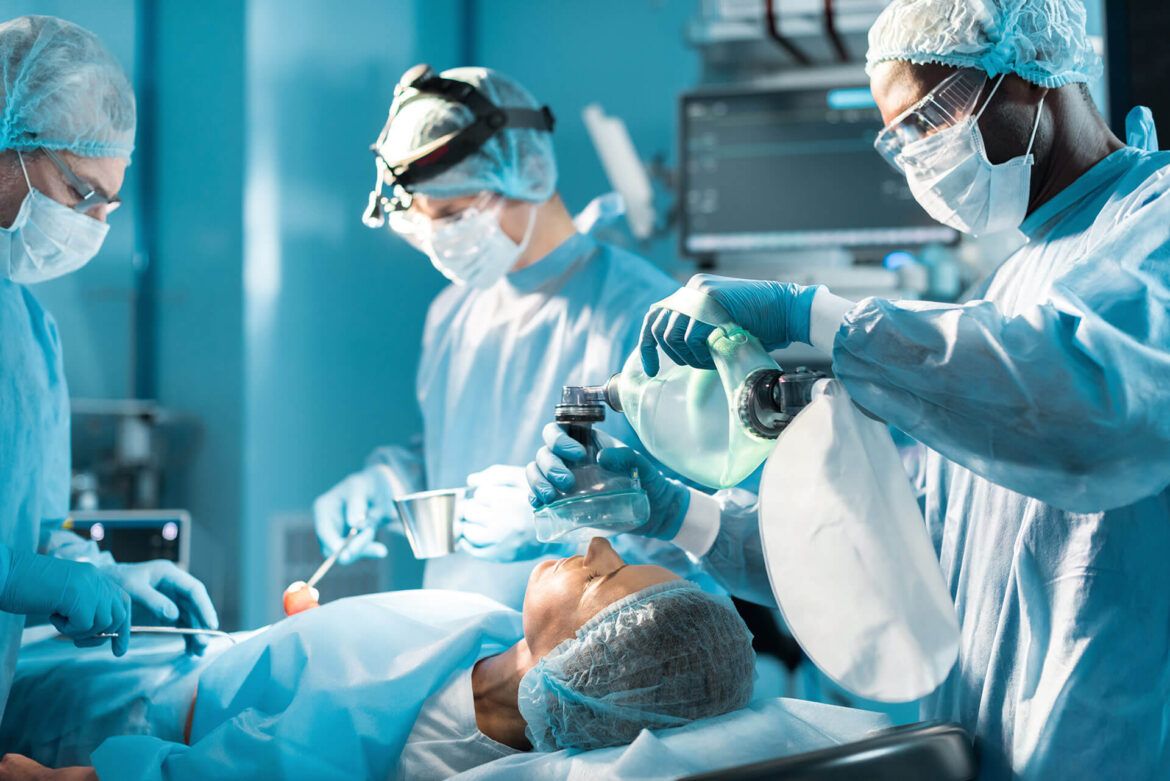
Challenges in OR Control Systems: The Critical Relevance of Efficient Integration
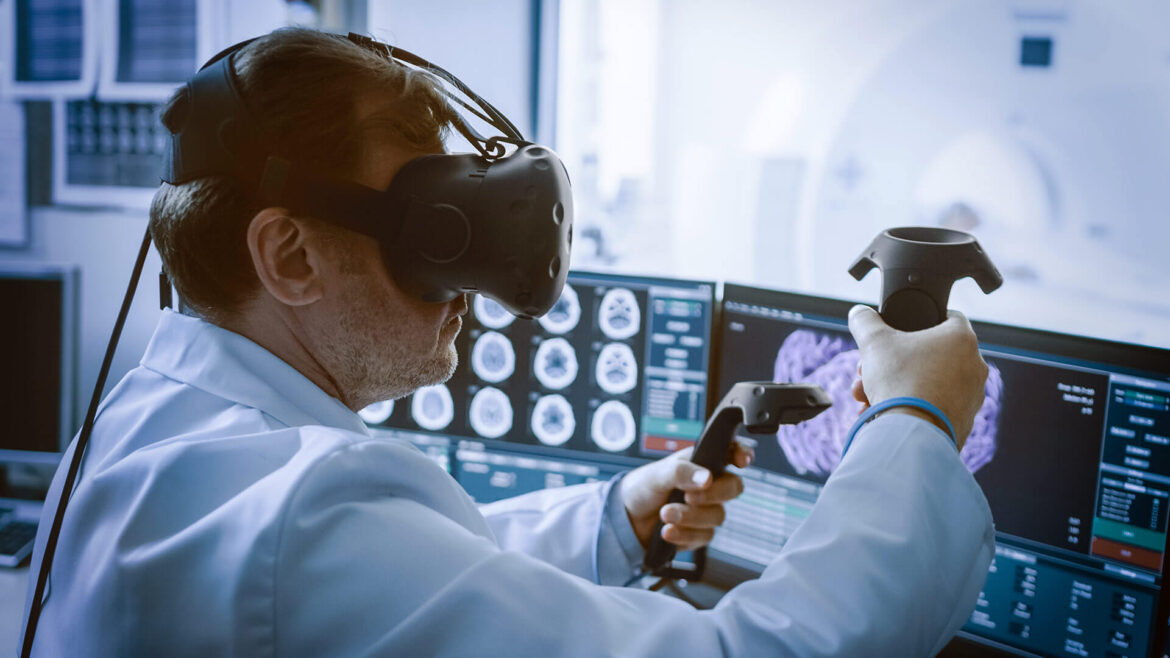
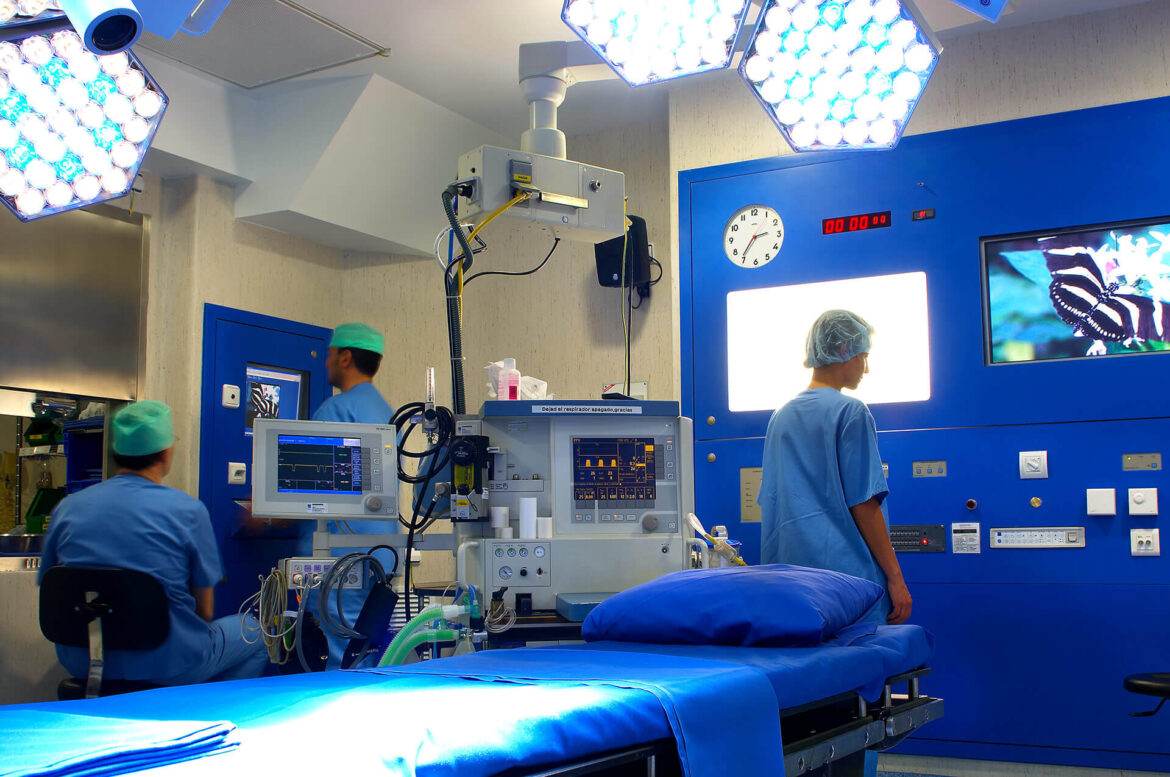
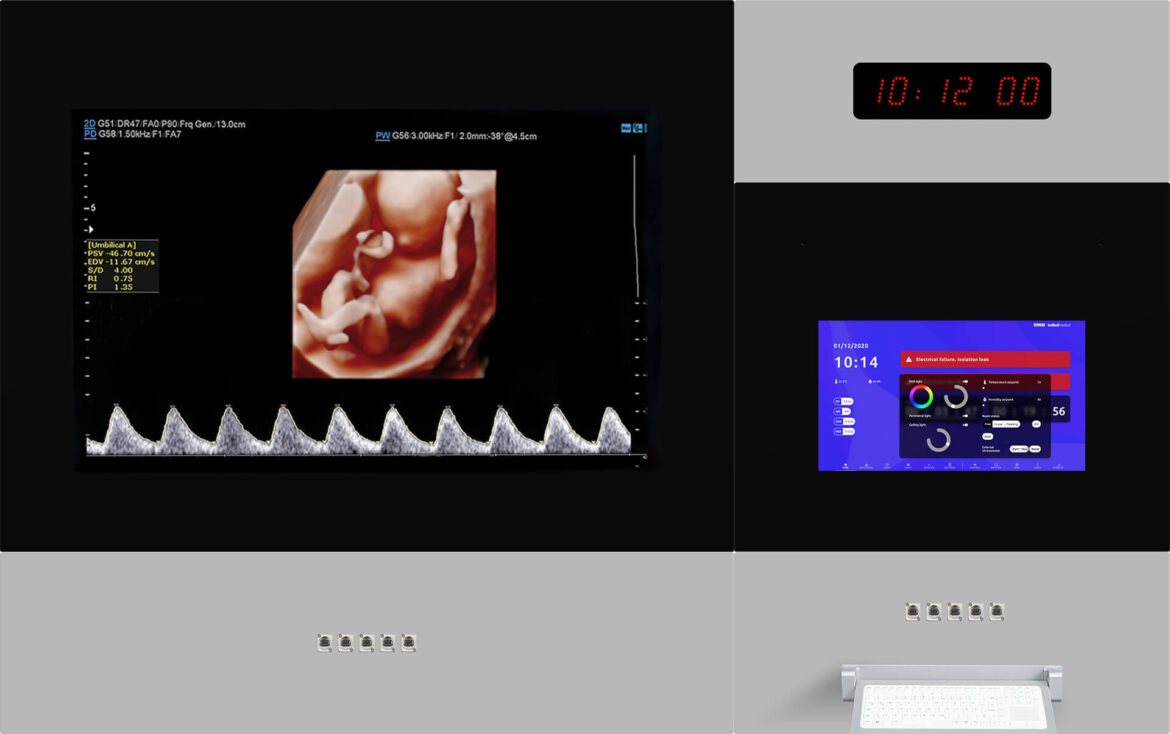
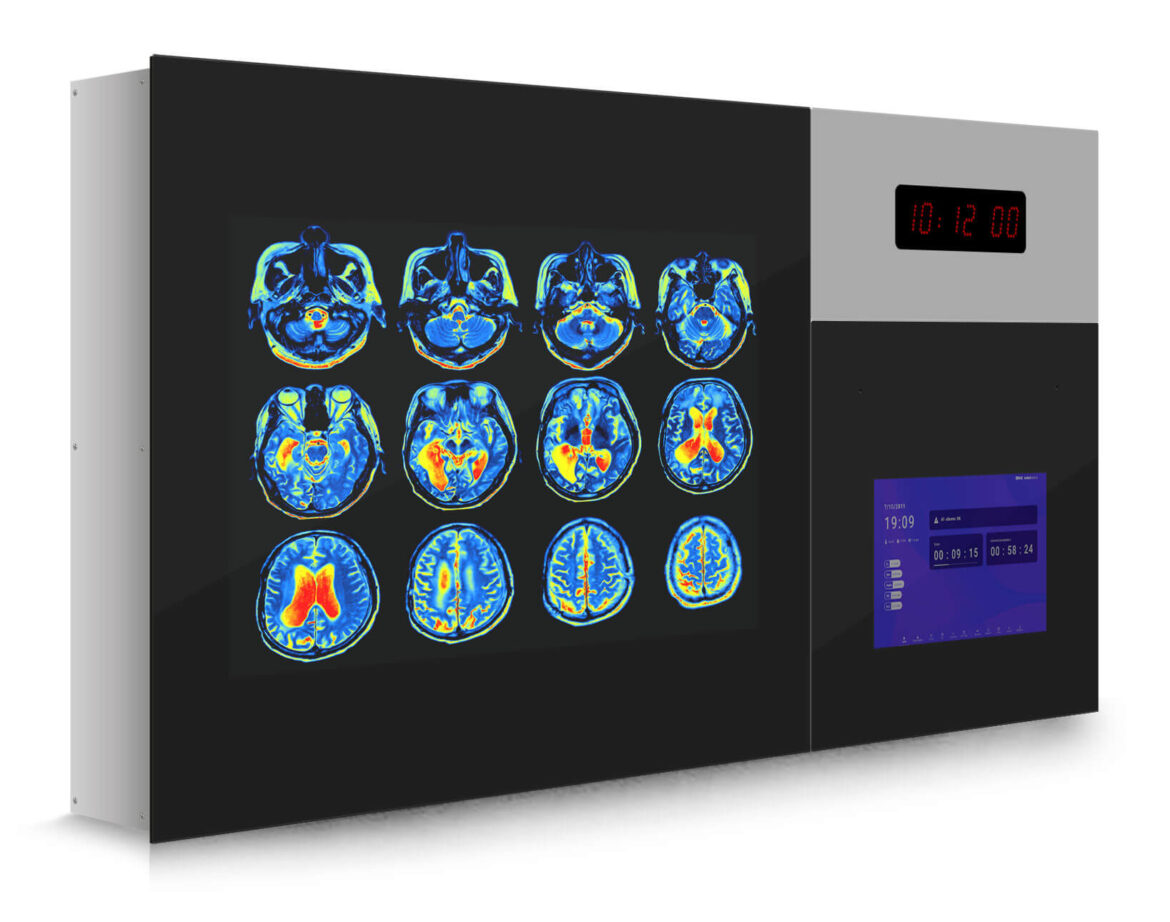
The introduction of advanced diagnostic and imaging technologies in operating rooms and intervention rooms has transformed these spaces into increasingly complex and crowded environments, filled with various medical devices and screens. In addition to tables and lighting, temperature regulations, time, numerous procedure screens, communication system monitors, etc… are rapidly being integrated into the hybrid operating room setup.
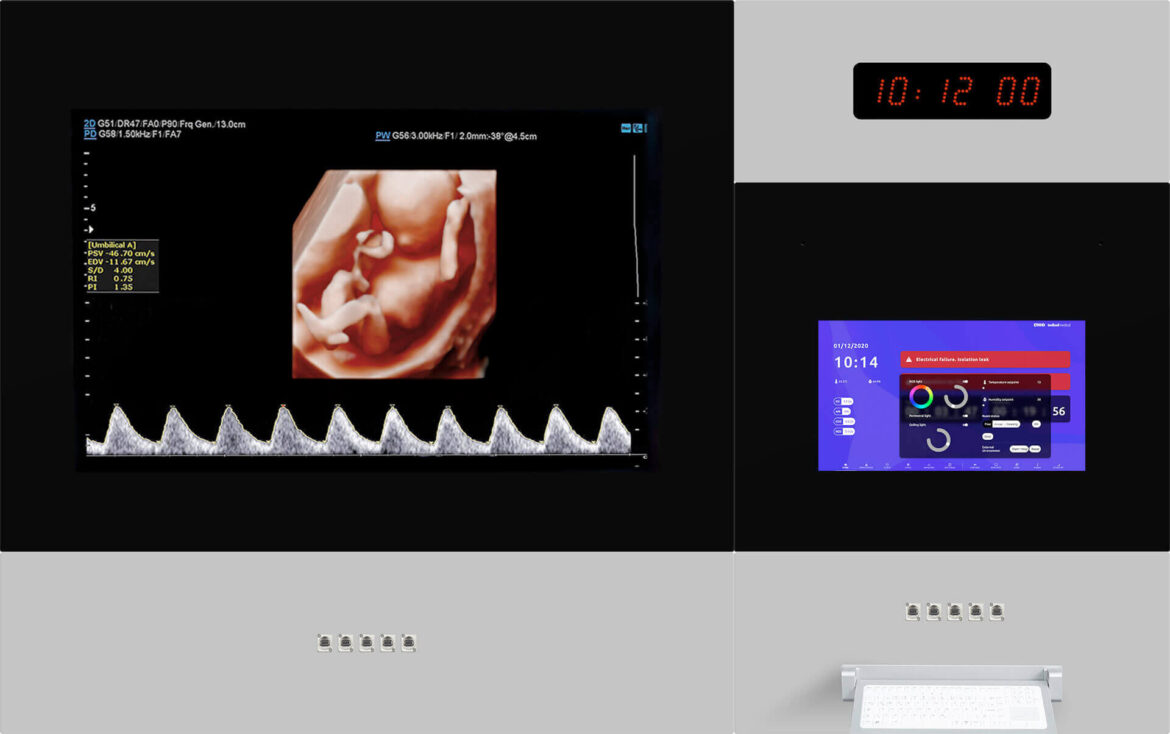
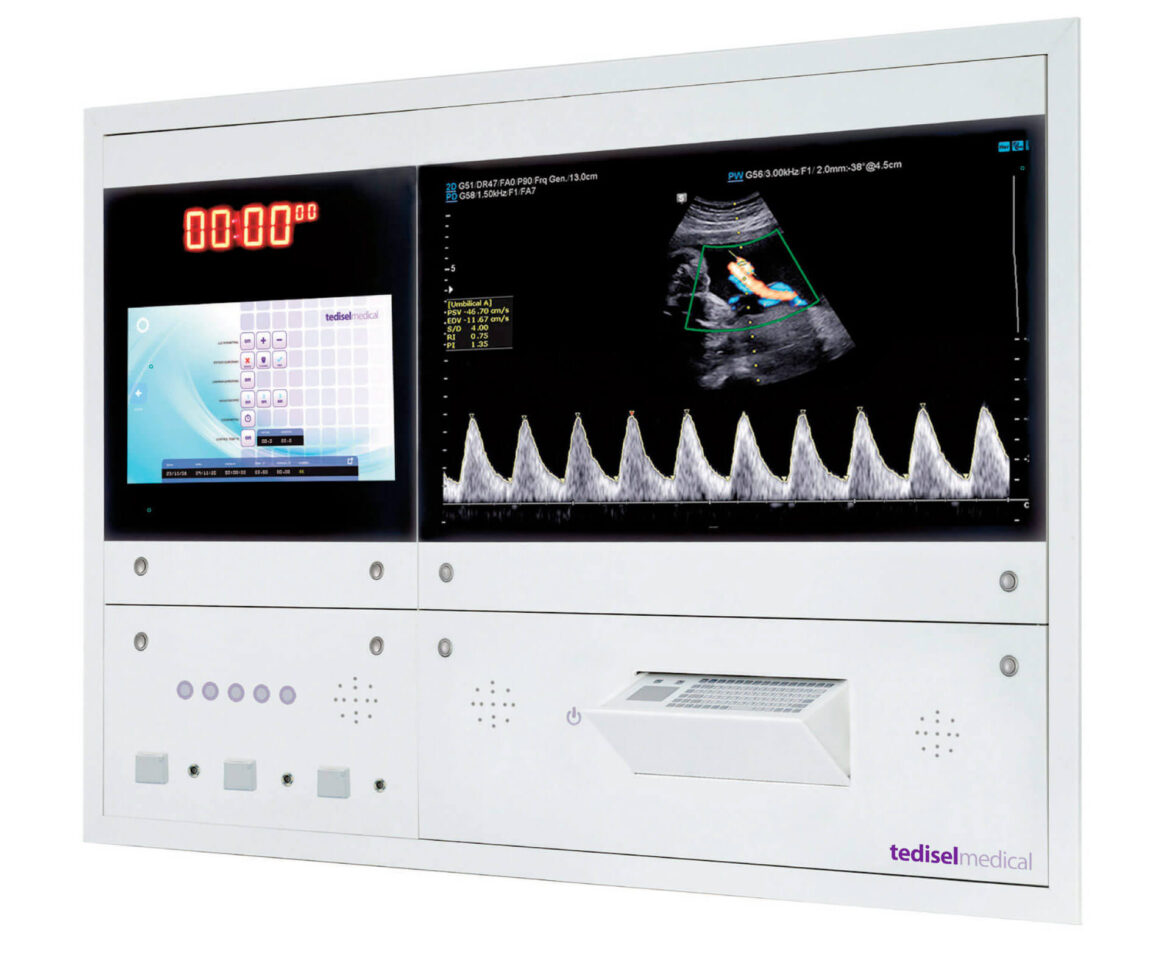
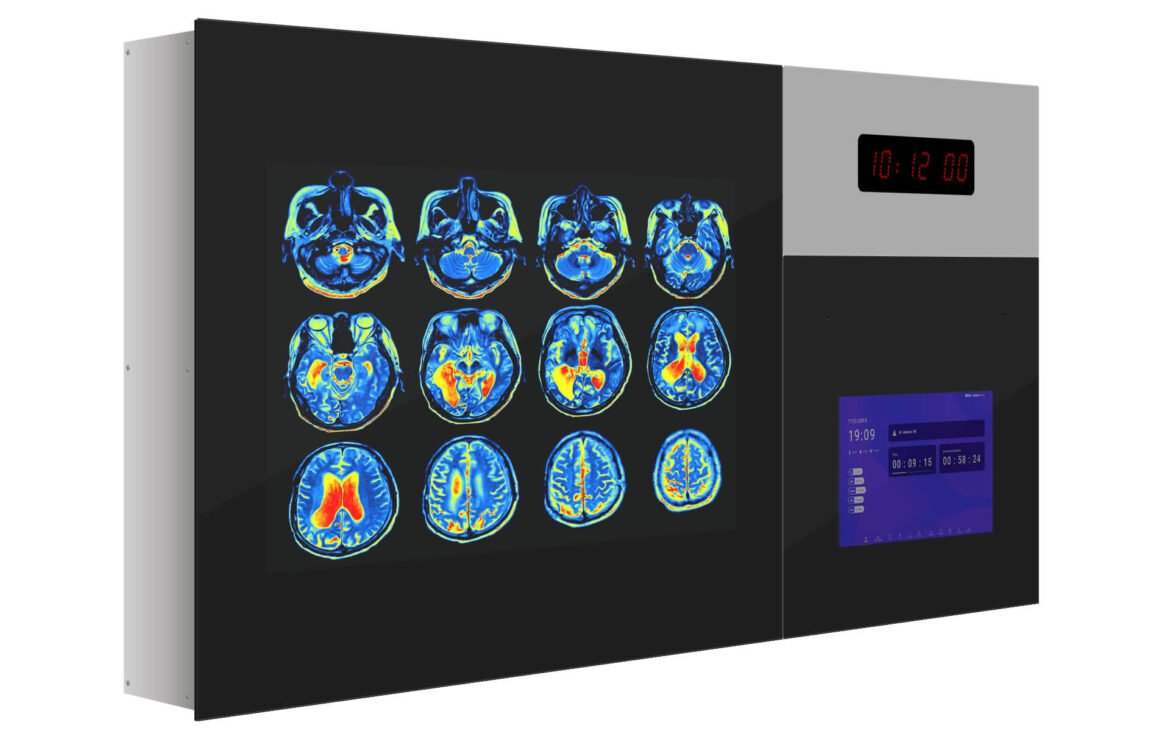
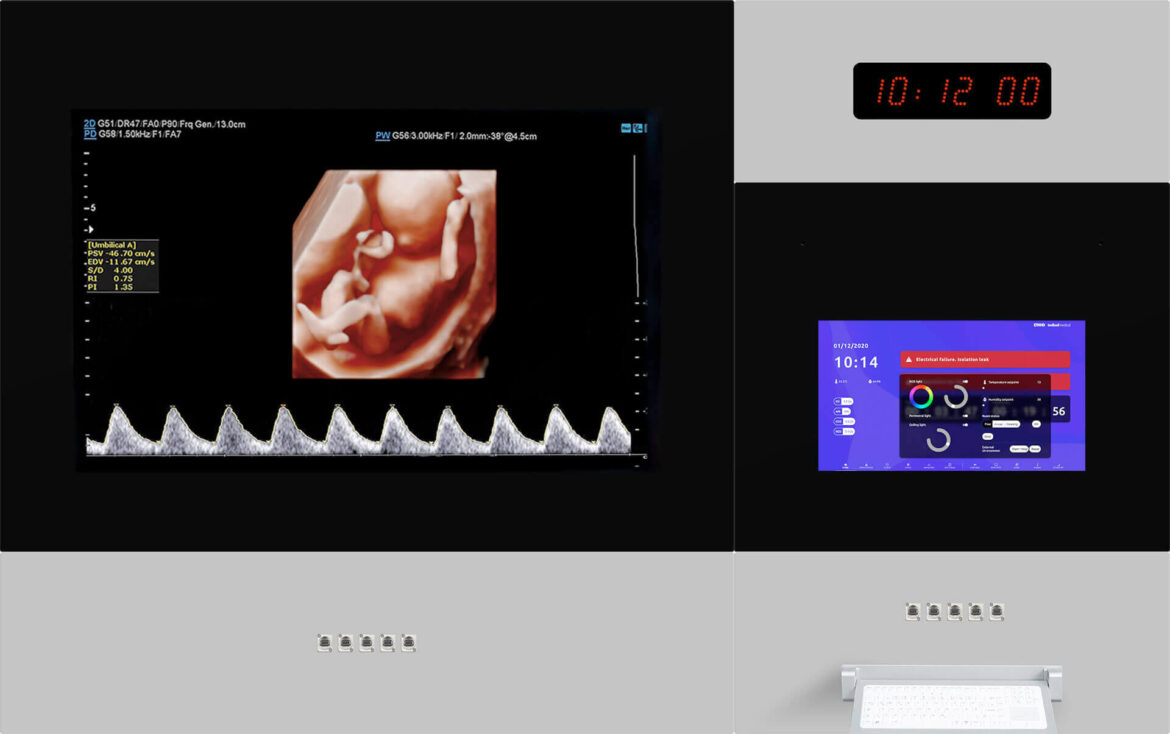
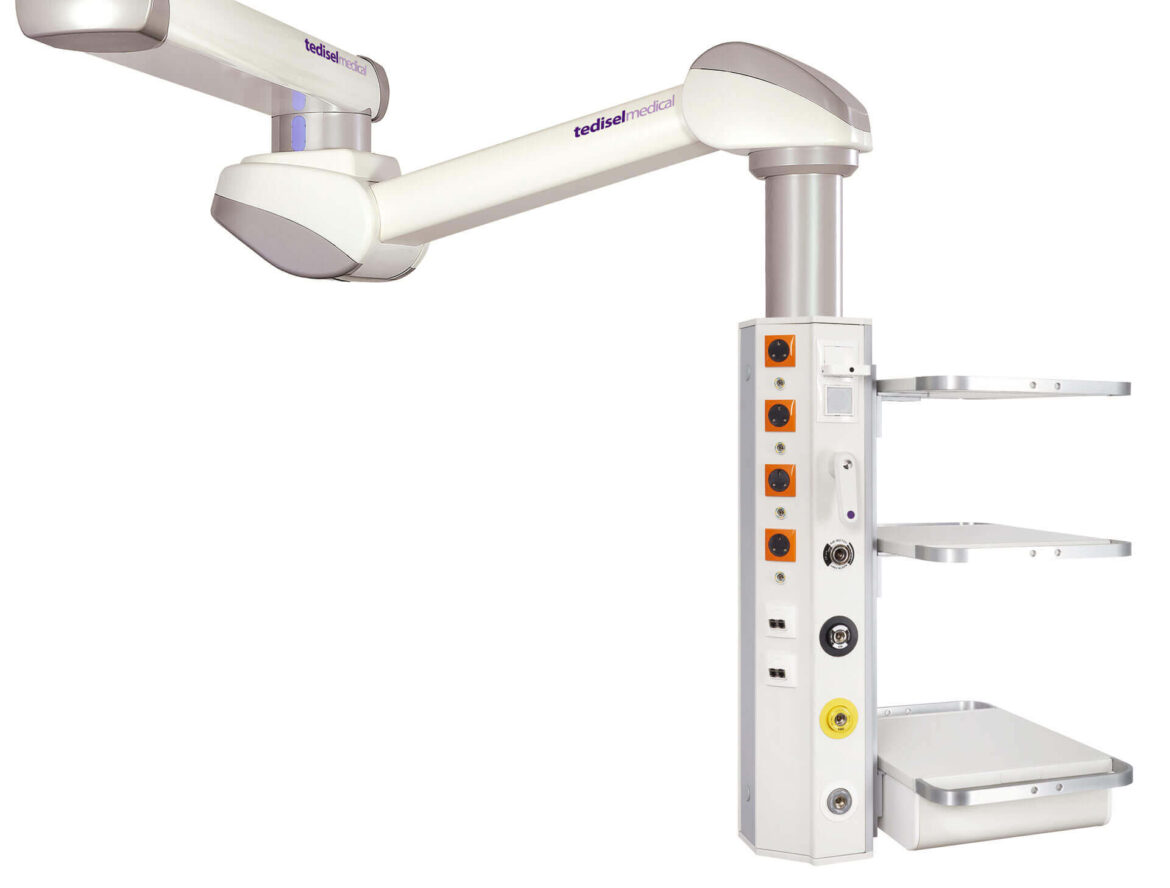
OR centralization systems like our Q-PANEL and DIAMOND models have been developed to simplify and optimize the operating room, unifying data and providing access to video and controls for all devices through a central panel. This allows perioperative staff to efficiently perform various tasks without the need to extensively move around the operating room, while ensuring optimal patient safety.
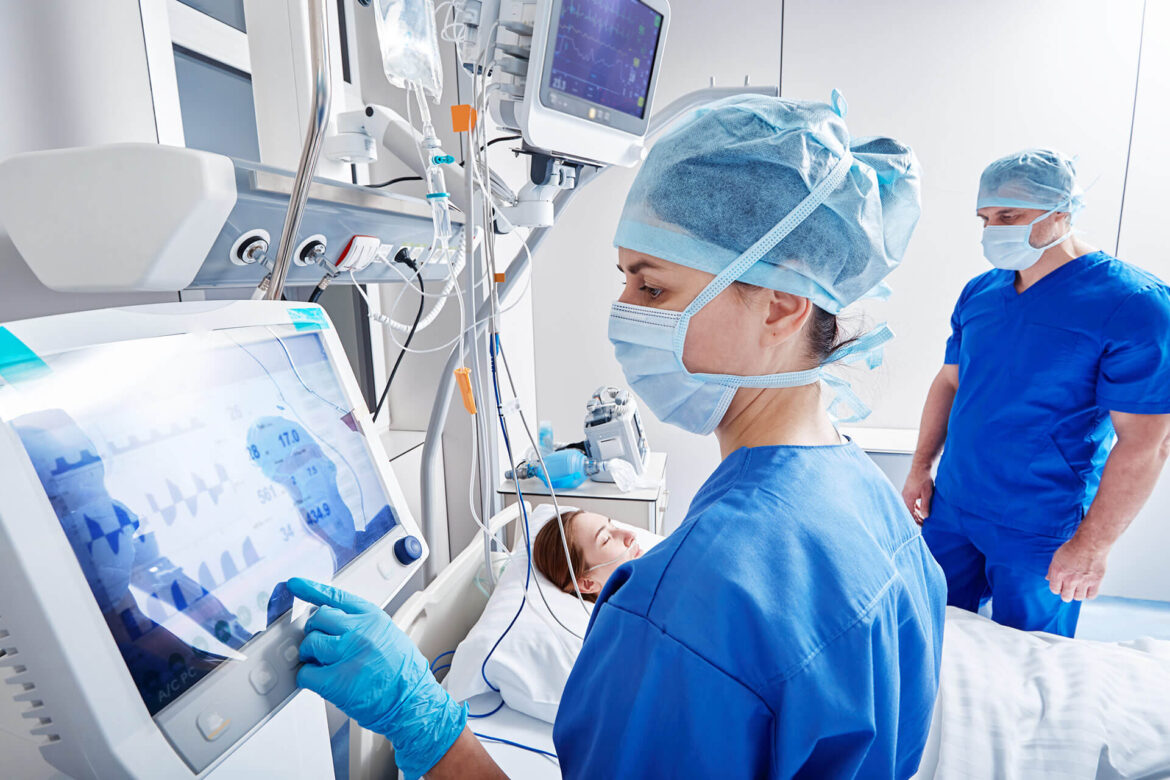
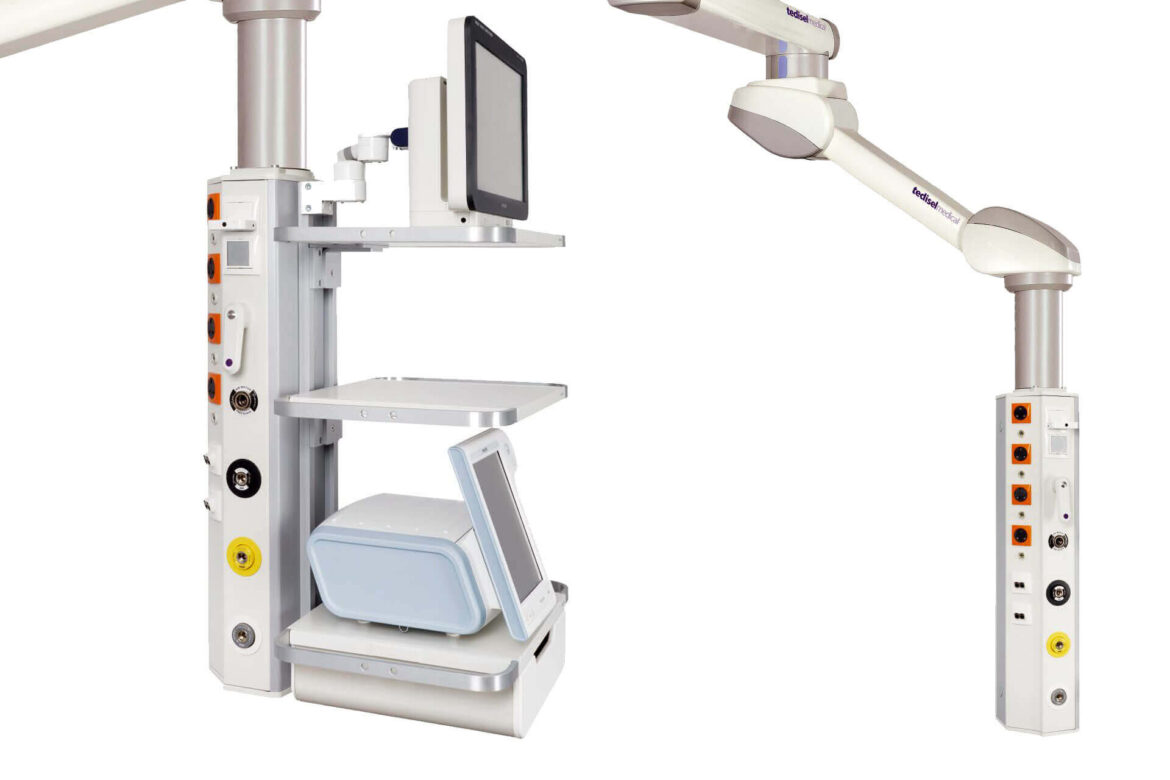
Surgical Optimization with Tedisel Technical Panels
The introduction of centralization systems in operating rooms with our innovative technical panels, such as the Diamond model and the Q Panel, brings notable benefits for medical work optimization. This approach allows the medical team to perform a greater number of interventions in the same room, eliminating the need to transfer material or personnel between different spaces, a common practice in conventional operating rooms. The advanced functionality of our panels significantly enhances safety, efficiency, ergonomics, and productivity in hybrid operating rooms.
Specific advantages include:
- Quick Access to Crucial Information: Our panels ensure quick access to crucial information (Hermes Software), without typical distractions or interruptions.
- Flexibility with Control: Q Panel controls allow easy room reconfiguration, adapting front doors to different elements, features, and accessories as per specific needs.
- Efficiency in Preparation and Cleaning: Simplification of equipment connection and disconnection between interventions streamlines preparations and cleaning.
- Customized Design for the Operating Room: The installation and arrangement of our equipment are meticulously designed to meet the specific needs of the operating room, providing solutions that enhance the overall effectiveness of the surgical process.

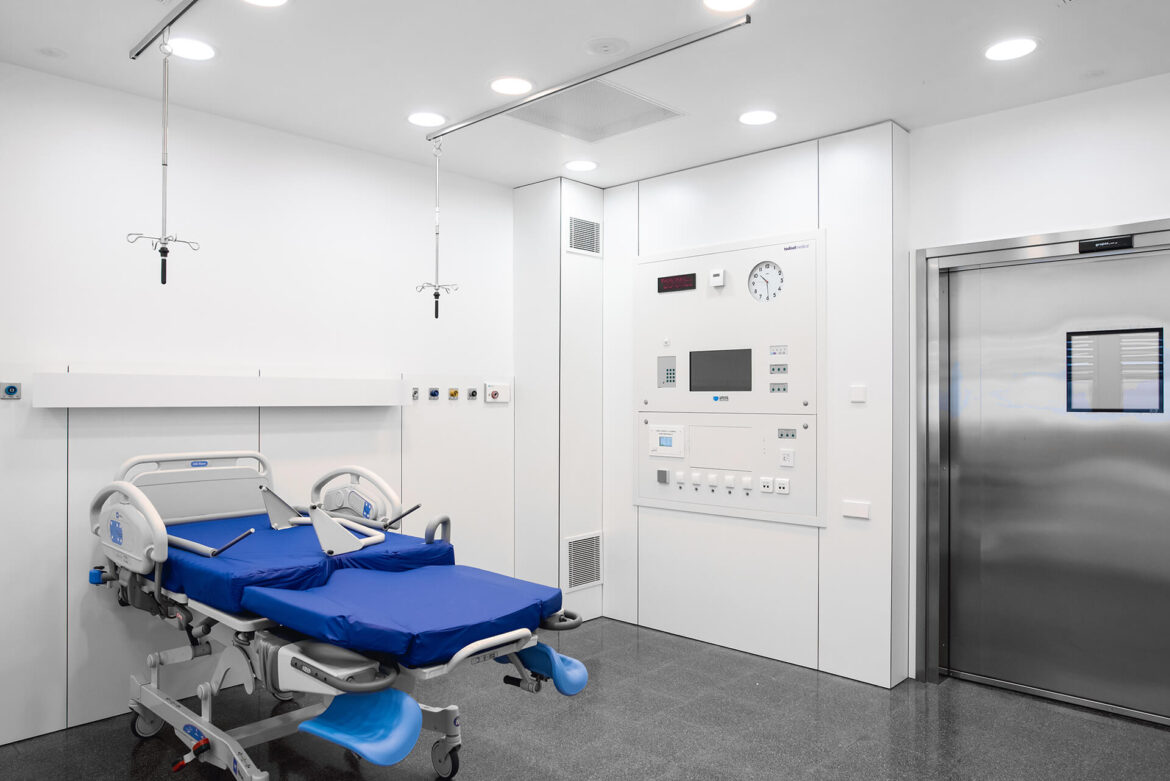
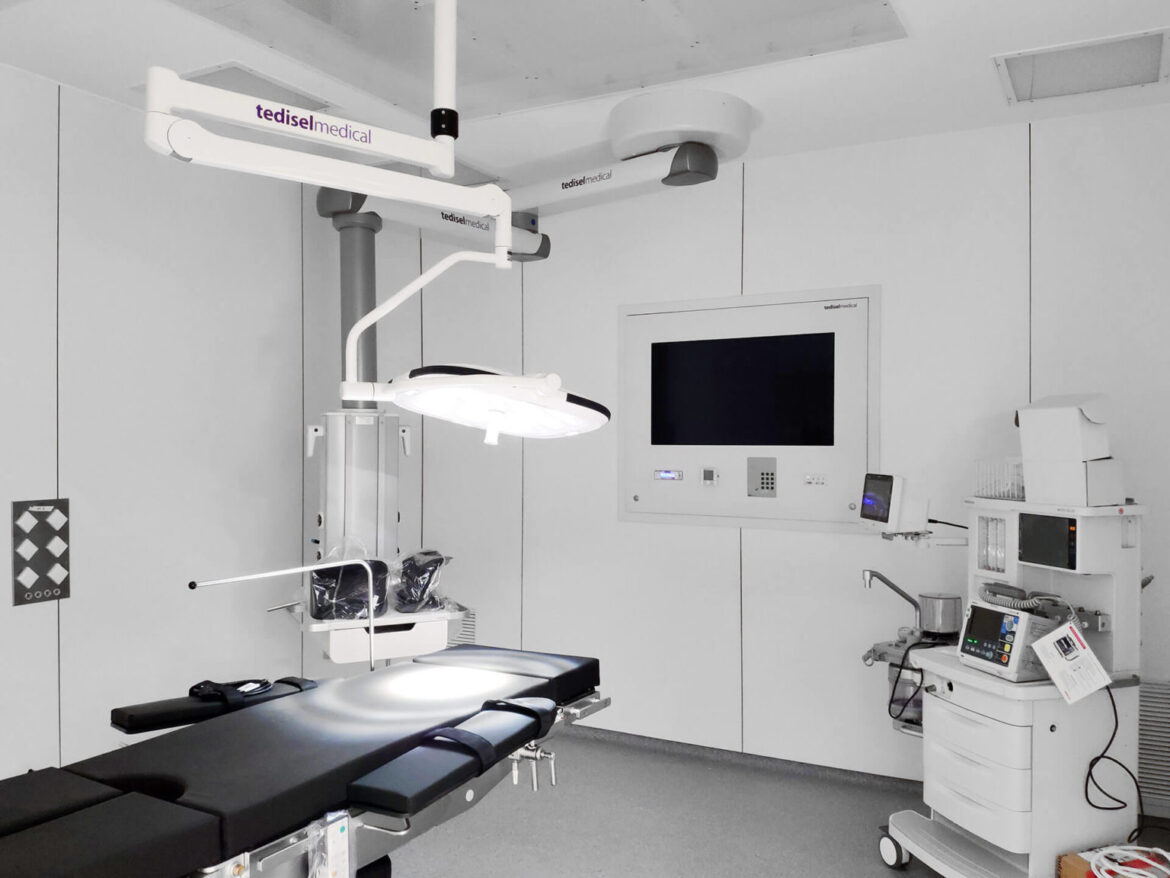
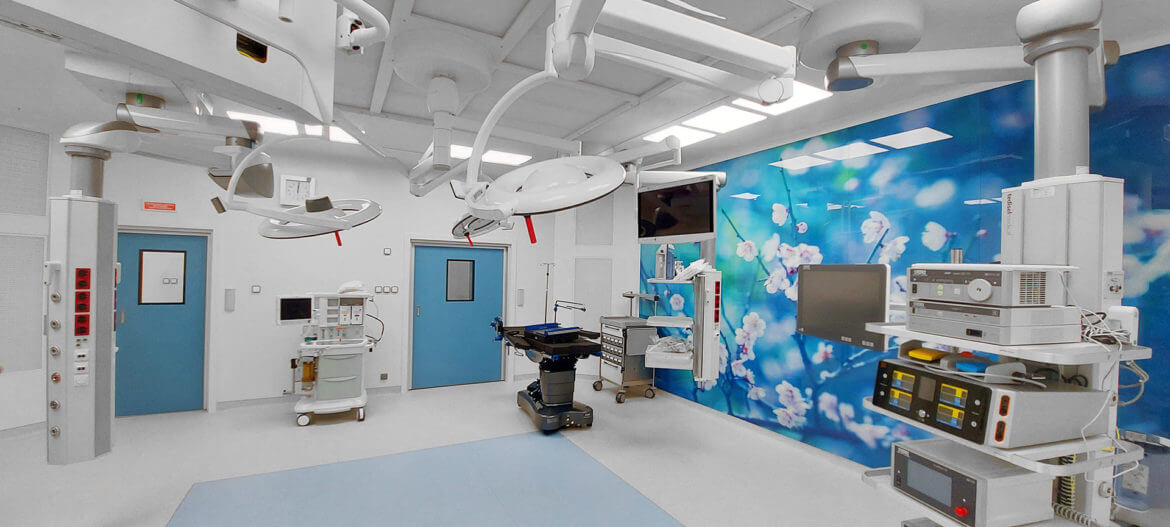
Hospital Distrital Beja (Portugal)
In summary, optimizing workflow in the OR and ICU emerges as a critical factor directly impacting patient safety and outcomes. Tedisel’s outstanding contribution in this field is manifested through a variety of meticulously designed models to adapt to the complexities of contemporary hospital environments. Tedisel’s implementation of advanced technologies not only simplifies procedures but also enhances the overall effectiveness of the surgical process, setting a standard for a future of more efficient and safer healthcare. Ultimately, Tedisel’s constant pursuit of excellence reflects its commitment to continuous improvement in patient care and the medical staff experience in the hospital environment.