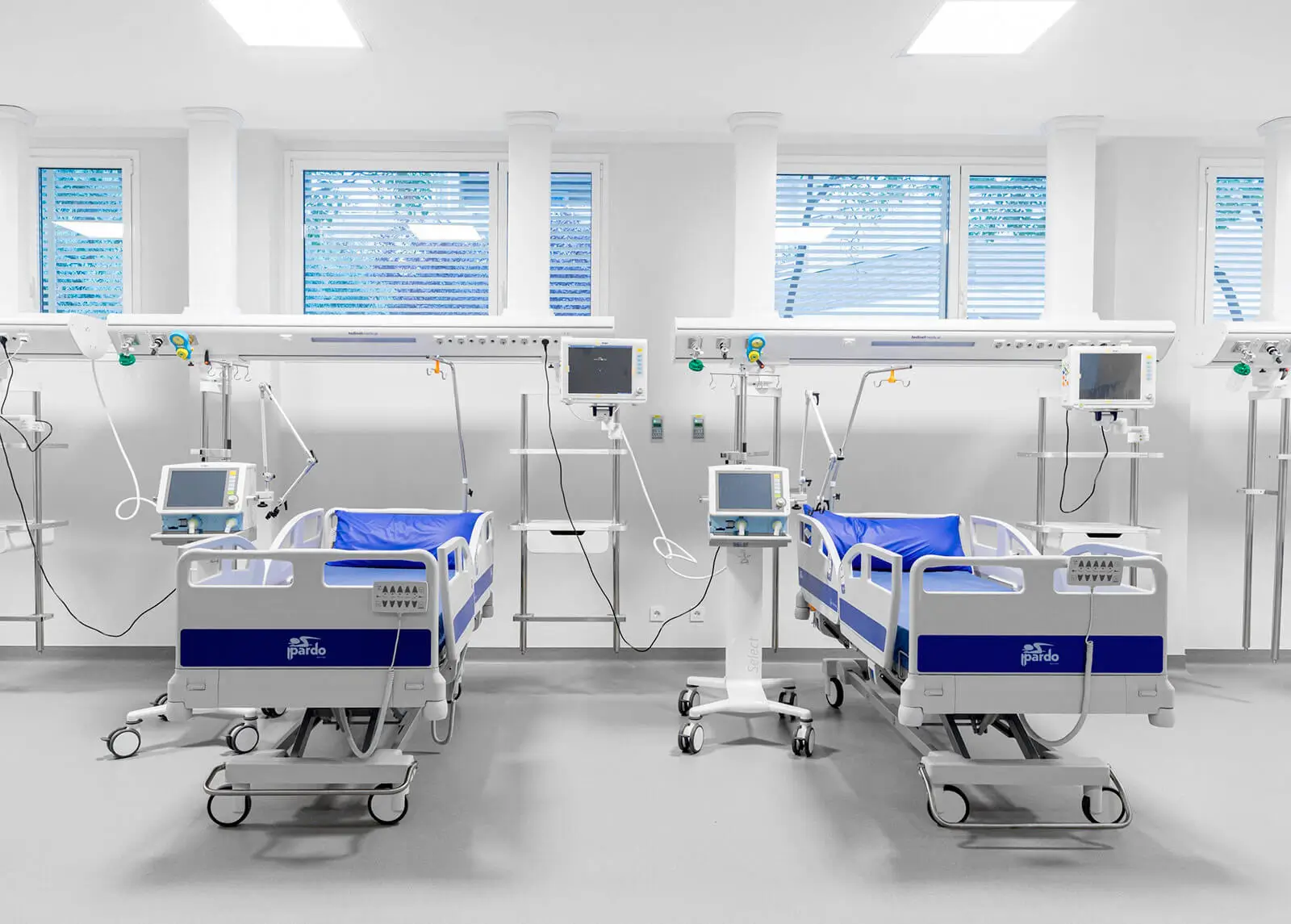
A smart ICU combines integrated equipment, clinical accessibility and an environment designed to respond quickly to high-complexity situations.
ICU hospital design has become a strategic element in modern healthcare architecture. Intensive Care Units are no longer just functional spaces. Today, they must operate as connected clinical ecosystems where every design decision directly affects patient safety, clinical efficiency and the working capacity of healthcare teams.
In this new context, the combination of advanced ICU equipment, connectivity, ergonomics and human-centered planning defines the real shift toward a smart ICU. The goal is not simply to add more technology, but to integrate it coherently so professionals can act with speed, precision and safety in highly demanding care environments.
The ICU of the future is not just a physical space. It is a clinical infrastructure designed to maximize outcomes, reduce risk and improve the care experience.
What is ICU hospital design?
ICU hospital design is the process of planning and organizing space, equipment, technical infrastructure and digital systems in intensive care units in order to improve patient safety, support clinical efficiency and help healthcare professionals work more effectively in high-complexity environments.
Evolution of ICU hospital design: from technical space to adaptive environment
For many years, ICU rooms were planned using static criteria: fixed layouts, independent devices and an organization model designed more to host technology than to optimize clinical work. However, rising care pressure, the growing complexity of treatments and the need for more resilient hospital environments have transformed this approach.
Today, ICU hospital design must respond simultaneously to multiple demands: rapid patient access, visual and functional continuity, system integration, reconfiguration capability and the reduction of interference. This evolution aligns with the approach promoted by the World Health Organization, which highlights the importance of the physical environment in patient safety and healthcare system resilience, as well as with the work of ECRI, focused on reducing clinical and organizational risks.
At the same time, this approach is aligned with the growing need to optimize care processes in critical environments, as discussed in the article on optimizing workflow and safety in critical care areas.
In addition, the recommendations of the Facility Guidelines Institute reinforce the need to design critical care areas where circulation, accessibility, equipment organization and adaptability operate as part of the same strategy. In other words, healthcare architecture can no longer be separated from clinical performance.
Hospital design is no longer a purely architectural issue. It is a direct tool for clinical and operational improvement.
Key elements of ICU hospital design
A modern ICU hospital design should integrate the following elements:
- Bed head units that centralize essential services.
- Ceiling supply units and suspended columns that provide 360-degree access around the patient.
- Digital integration systems for monitoring, control and data visibility.
- Medical gas and electrical infrastructure organized for fast, safe intervention.
- Ergonomic layouts designed around healthcare staff workflows.
- Human-centered planning that supports comfort, orientation and reduced environmental stress.
Advanced ICU equipment: integration as the operational foundation
The real performance of an ICU depends to a great extent on how equipment is distributed and integrated. When supply points, support systems and control elements are scattered or overlap, the chance of error increases, workflows become more difficult and the care team loses valuable time during intervention.
For this reason, advanced ICU equipment is no longer understood as a set of isolated devices, but as a comprehensive solution that serves clinical operations.
Bed head units: order, centralization and safety
Bed head units make it possible to gather medical gases, electrical outlets, connectivity, lighting and other critical resources on a single clinical front. This approach improves room organization, reduces the risk of incorrect connections and provides a clearer reading of the environment during procedures.
Within this model, Tedisel Medical offers solutions such as Adonis, designed for limited space and critical care areas where compactness and functionality are essential.
A well-designed bed head unit does not simply improve the arrangement of services. It also simplifies the daily work of nurses and intensivists by centralizing points of use and making access more intuitive. That operational clarity reduces repetitive friction, saves time during routine tasks and helps create a safer and more efficient care environment. In intensive care, those seemingly small gains have a direct impact on quality of care.
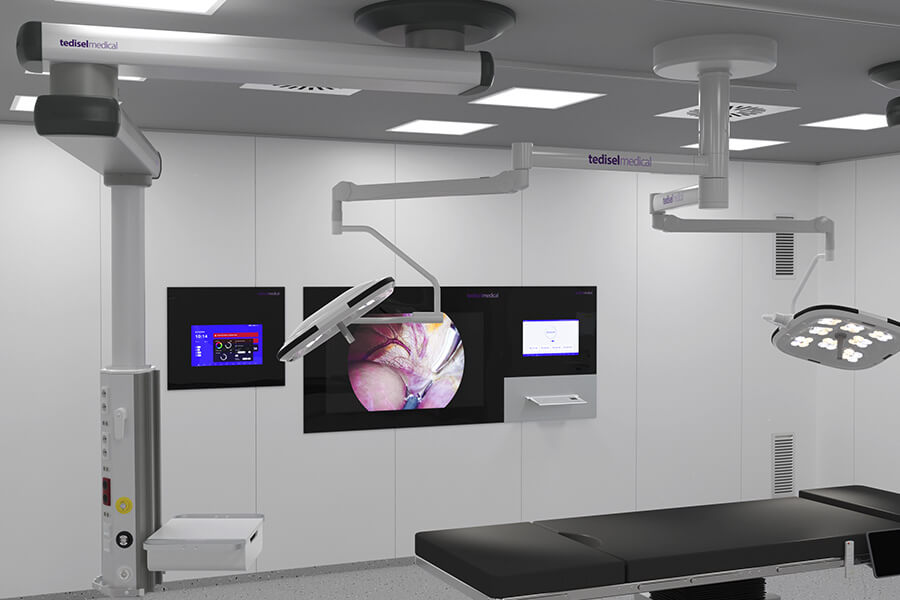
Suspended units and hospital columns: accessibility and real flexibility
In high-complexity critical care areas, freeing the floor is a clear functional advantage. Suspended systems help organize equipment above the intervention area, clear the care zone around the bed and support staff mobility.
This is why solutions such as Atlas, a ceiling supply unit created for critical areas, provide a strong operational base for accessibility, ergonomics and adaptability.
In the same direction, S-Column follows a logic that is especially relevant in ICU rooms and operating theatres. It brings equipment closer to the point of use, improves the working area and allows a more natural interaction between the clinician and the technical environment. The ability to organize monitors, pumps, accessories and supplies on an accessible structure has a direct effect on response times and on reducing unnecessary movement.
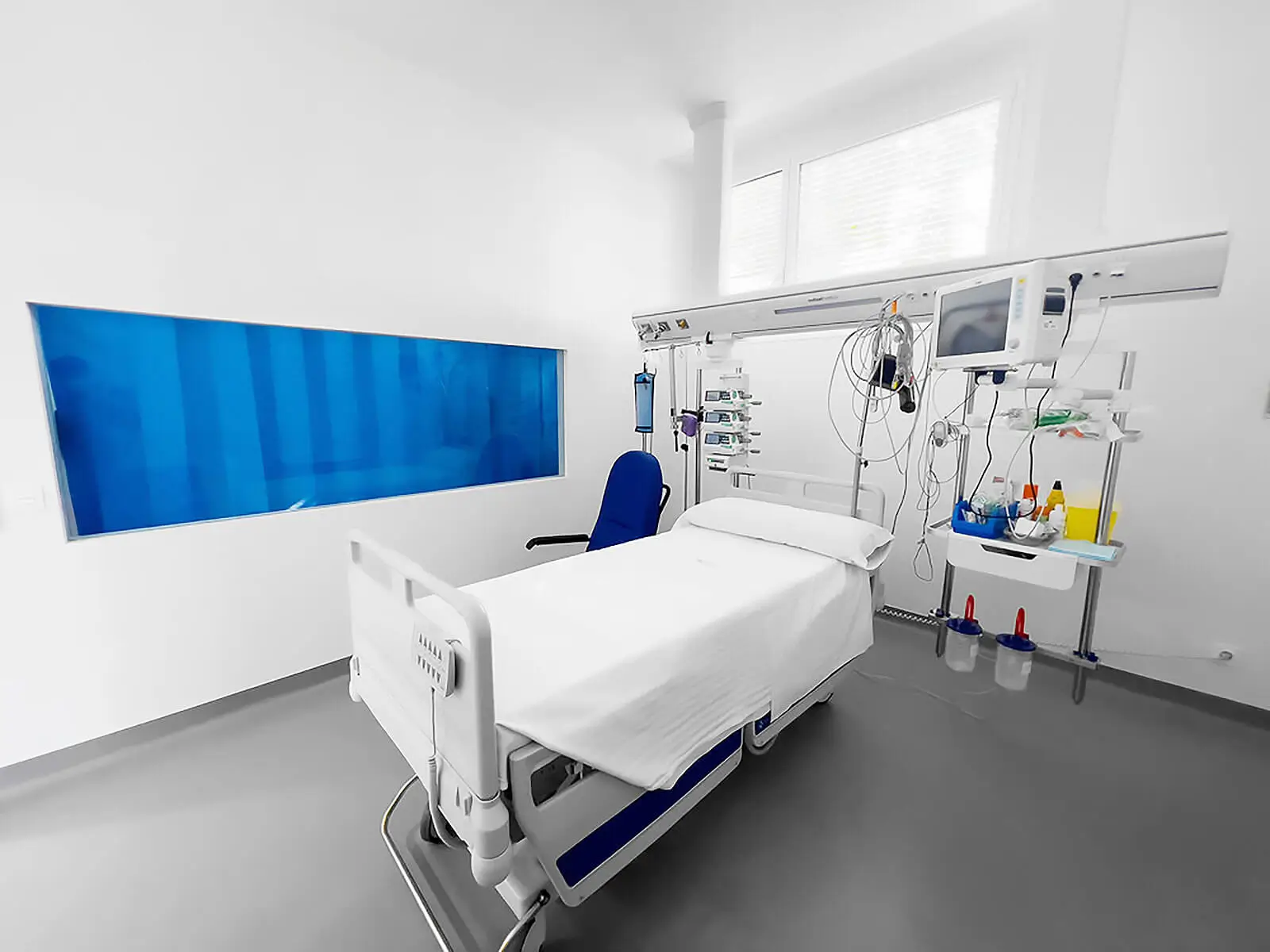
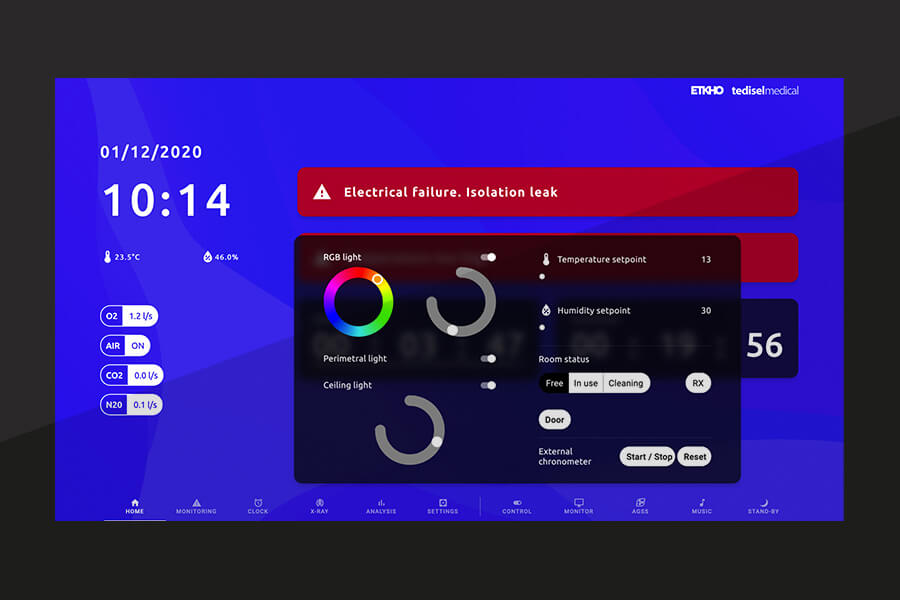
Digital integration and environmental control
The move toward a smart ICU also requires an environment capable of centralizing information and facilitating clinical coordination. In this area, Tedisel integrates tools such as HERMES, designed for digital control and integration of the clinical environment, and solutions such as Q Panel, which strengthen the logic of centralized management, control and operational visibility.
This integration approach is not exclusive to the ICU. It forms part of a broader strategy for the hospital’s critical areas. In the surgical environment, for example, technical panels in operating theatres apply the same logic of centralized control, improving clinical environment management and reinforcing patient safety.
When technology stops working in isolation and becomes part of the care workflow, the result is a more legible, predictable and safer ICU. Connectivity is no longer an added value. It is part of the critical infrastructure that supports real-time decision-making.
Technology integration turns the ICU into an environment where information, equipment and clinical work flow without unnecessary friction.
Smart ICU: digitalization, data and clinical anticipation
Talking about a smart ICU also means understanding the evolution toward connected digital environments, where data, continuous monitoring and system integration make it possible to anticipate clinical situations. This transformation is part of a broader shift toward the digital hospital, as explained in the article on the digital ecosystem in the ICU.
In this model, device connectivity, continuous monitoring, alert systems and the centralization of relevant clinical information work together. This approach helps reduce cognitive load for staff, lowers information fragmentation and supports faster and better-informed decisions. The final objective is not to add complexity, but to turn clinical complexity into a clearer and safer operation.
Digitalization should not be separated from physical planning. A well-designed critical care environment is one where patient access, equipment layout and support-system visibility reinforce one another. For that reason, ICU design and technology strategy should be developed as a single project.
Clinical ergonomics: designing to intervene better
One of the most common mistakes in planning critical care areas is to treat ergonomics as a secondary issue or a matter of comfort alone. In reality, clinical ergonomics directly affects the precision of interventions, staff fatigue, response speed and error reduction.
Every unnecessary movement, every poorly positioned connection point and every physical barrier around the patient adds friction to an already demanding operation.
The combination of bed head units, suspended systems and centralized control tools helps create an environment where healthcare professionals can work more naturally. Wide access around the patient, equipment placed in the zone of use, immediate visibility of relevant information and a clear distribution of functions improve both clinical performance and patient safety.
This ergonomic logic is especially relevant in periods of high care intensity, when reaction times become shorter and multidisciplinary coordination depends heavily on available space and environmental clarity.
Real projects: Tedisel solutions applied to critical care areas and ICU environments
Hospital HC Miraflores
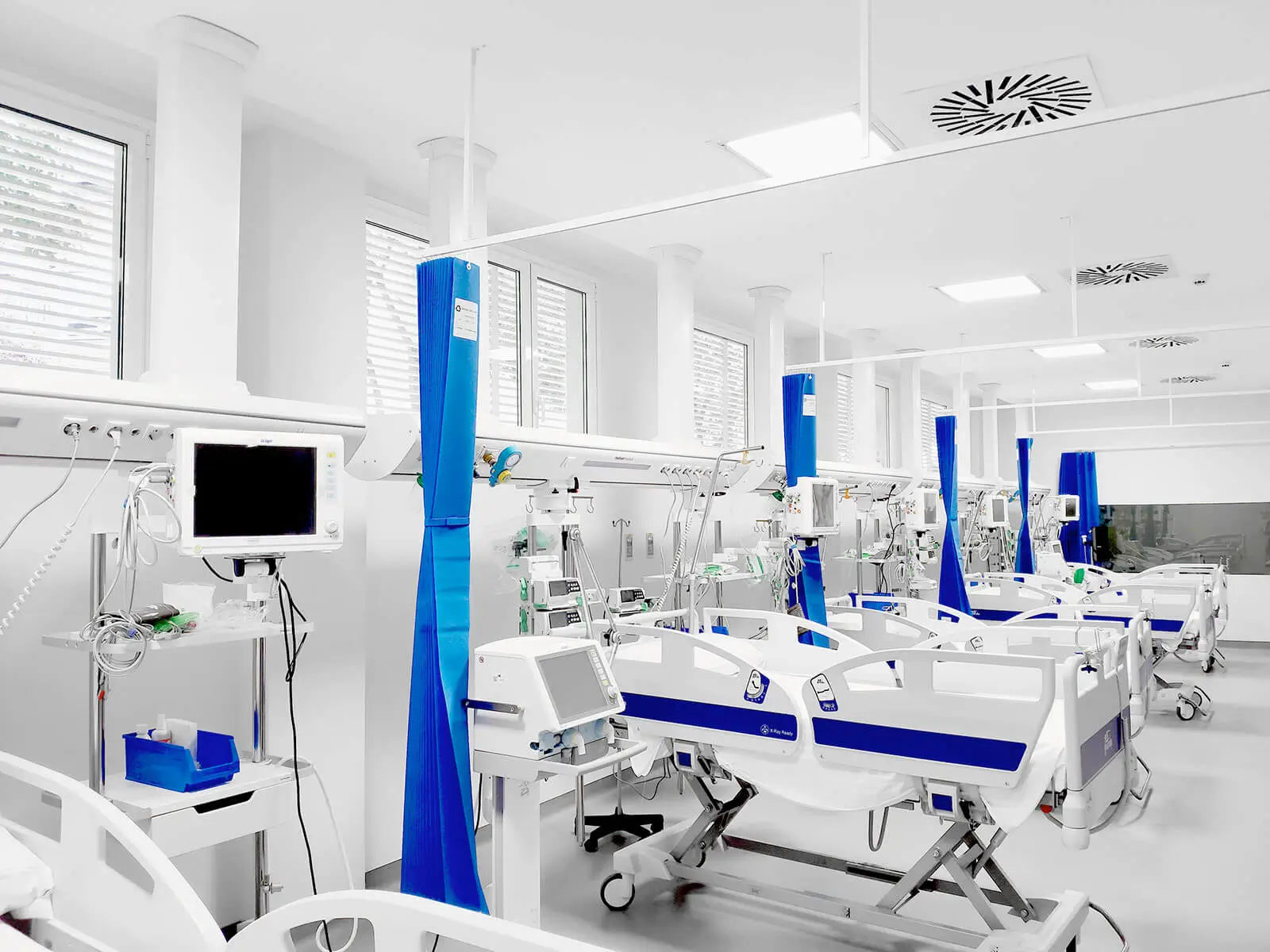
The project at Hospital HC Miraflores is especially useful for understanding how a coherent equipment strategy takes shape in a contemporary hospital. On the project page, Tedisel Medical links this installation to solutions such as Adonis, Atlas and Q Panel, among others.
From the perspective of ICU hospital design, this project is relevant because it shows a strong combination of wall-mounted solutions, suspended systems and control elements. In other words, it follows an integration logic that fits the needs of critical care areas where environmental organization, accessibility and operational continuity are decisive.
Beyond the specific product range, the real value lies in the planning approach: structuring the clinical space so equipment supports care flow instead of interrupting it. This type of implementation helps reduce visual and technical clutter, improves the functional readability of the room and creates more efficient environments, especially when patient care requires multiple devices and constant coordination between professionals.
Hospital General Universitario de Castellón
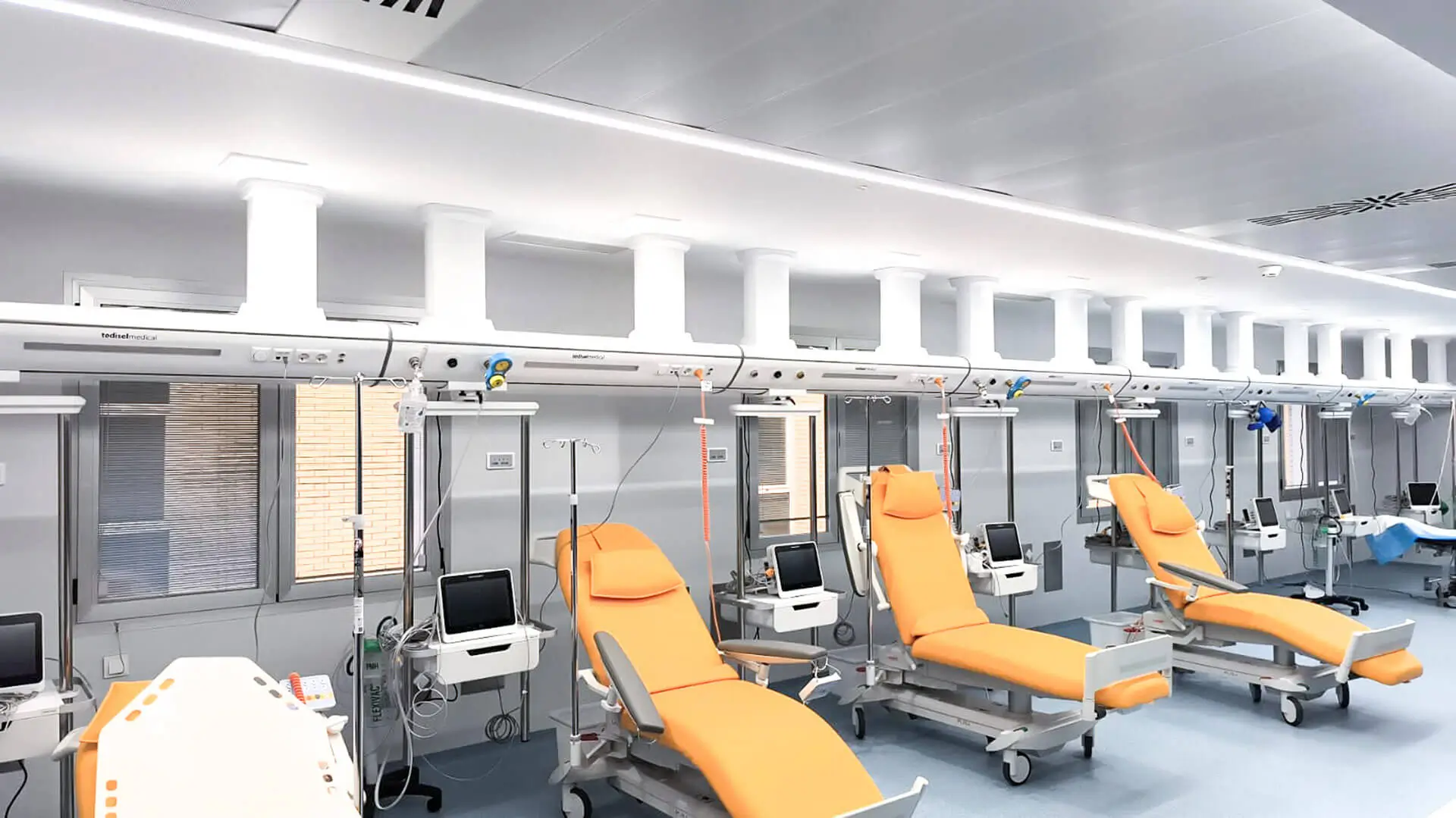
Hospital General Universitario de Castellón offers an even more direct case for this article because the project information itself mentions the installation of Atlas suspended systems in surgical areas and ICU spaces. That detail makes the project particularly useful for connecting design, product and real application in critical care environments.
The use of a ceiling-mounted supply unit responds to several essential ICU needs: freeing the floor, bringing equipment closer to the point of use, facilitating access to the patient and enabling a cleaner room configuration. All of these factors improve team mobility, intervention speed and the reduction of interference during complex procedures.
Taken together, both projects reinforce one central idea: an efficient ICU does not depend only on the technological level of the equipment, but on how that equipment is integrated into the room, the clinical workflow and the hospital’s operational strategy.
Humanization in ICU hospital design
The integration of technology and efficiency should not distance the ICU from a more human approach to care. On the contrary, advanced planning makes it possible to improve lighting, visual order, environmental comfort and spatial perception. In critically ill patients, where stress, disorientation and overstimulation can worsen the care experience, a better-designed environment also creates clinical value.
Humanization is not a decorative layer added at the end of the project. It is a strategic dimension that must coexist with technology, functionality and safety. When the space reduces visual noise, improves environmental clarity and communicates calm, the effect on patients, relatives and professionals is clearly positive.

Conclusion: why ICU hospital design is already strategic
The future of ICU hospital design depends on integrating technology, ergonomics, connectivity and equipment organization into a single clinical ecosystem. The real transformation does not lie only in adding more devices, but in creating environments where every element contributes to safer, faster and more effective care.
Solutions such as Adonis, Atlas, S-Column, HERMES and Q Panel show how this vision is already becoming reality in Tedisel Medical projects. In a sector where every second and every decision matter, hospital design has stopped being a passive frame and has become a true driver of healthcare improvement.
Today, hospital design is a strategic tool for saving lives, optimizing processes and preparing critical care areas for the future.
Frequently asked questions about ICU hospital design
What should modern ICU hospital design include?
Modern ICU hospital design should include advanced clinical equipment, fast patient access, data connectivity, ergonomic planning for healthcare staff and solutions that improve safety, operational efficiency and the humanization of the care environment.
Why are bed head units and suspended columns important in an ICU?
Bed head units and suspended columns help centralize essential services, reduce clutter, improve access to the patient and support a safer and more efficient workflow. In critical care, these advantages have a direct impact on response times and clinical organization.
What are the main benefits of a smart ICU?
A smart ICU improves real-time visibility, supports faster decision-making, reduces operational errors and connects equipment, data and professionals in a more coordinated care environment.
How does ICU hospital design improve patient safety?
ICU hospital design improves patient safety by reducing environmental friction, organizing equipment more clearly, facilitating intervention and making the clinical space easier to understand and use under pressure.
Which Tedisel Medical solutions are especially relevant for ICU planning?
Solutions such as Adonis, Atlas, S-Column, HERMES and Q Panel are especially relevant because they help centralize services, improve accessibility, integrate digital control and support a more efficient critical care environment.