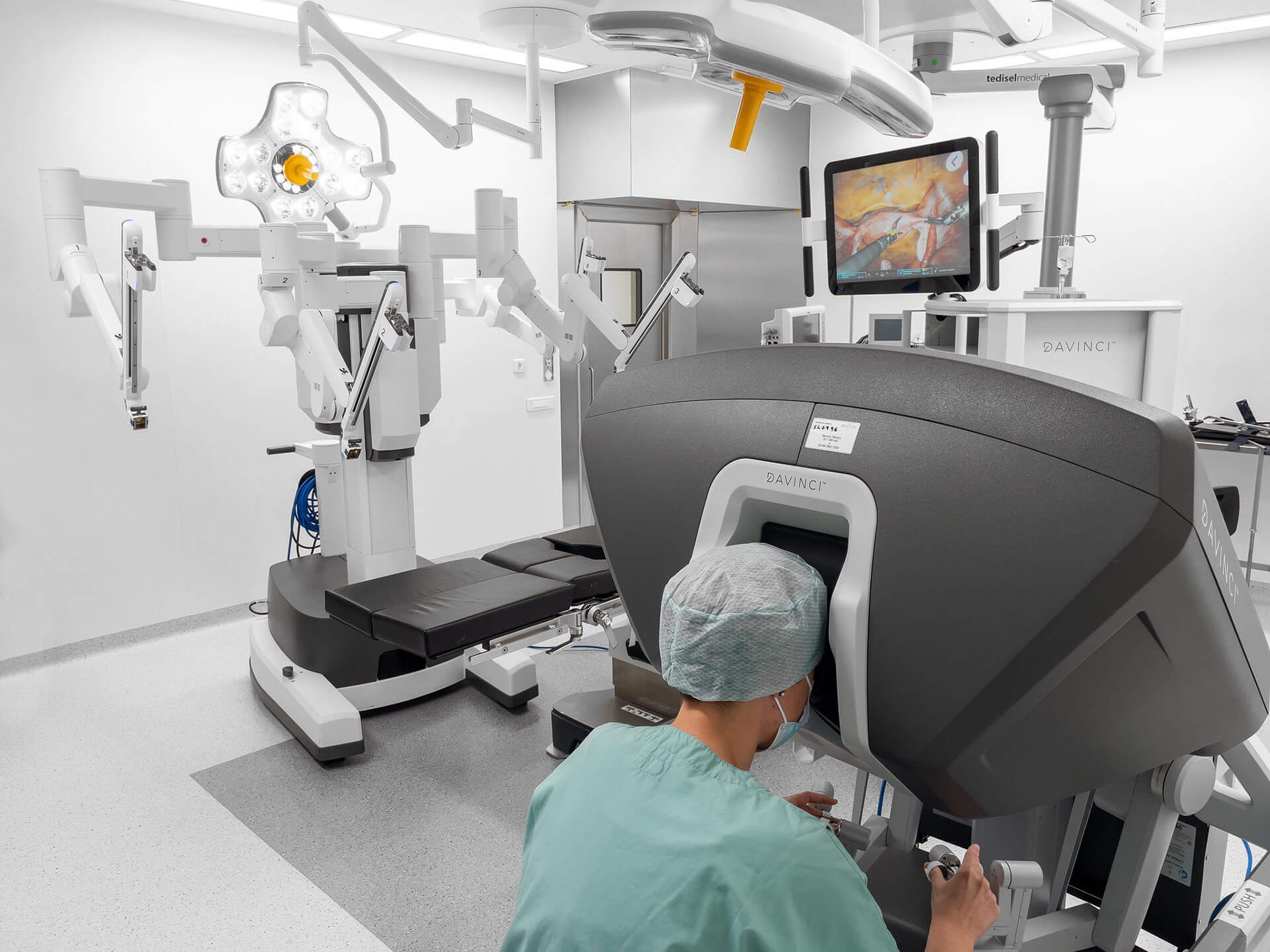
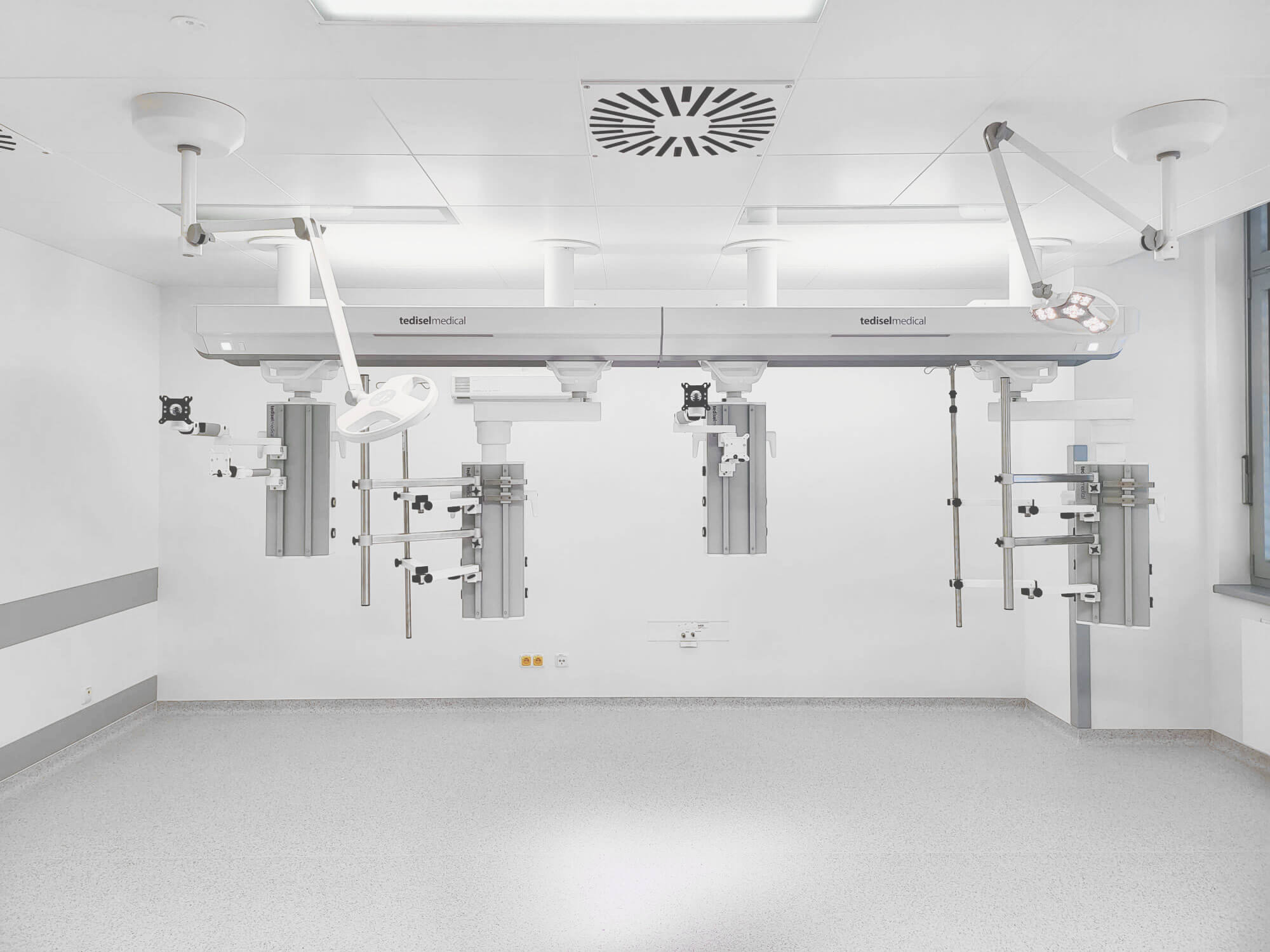
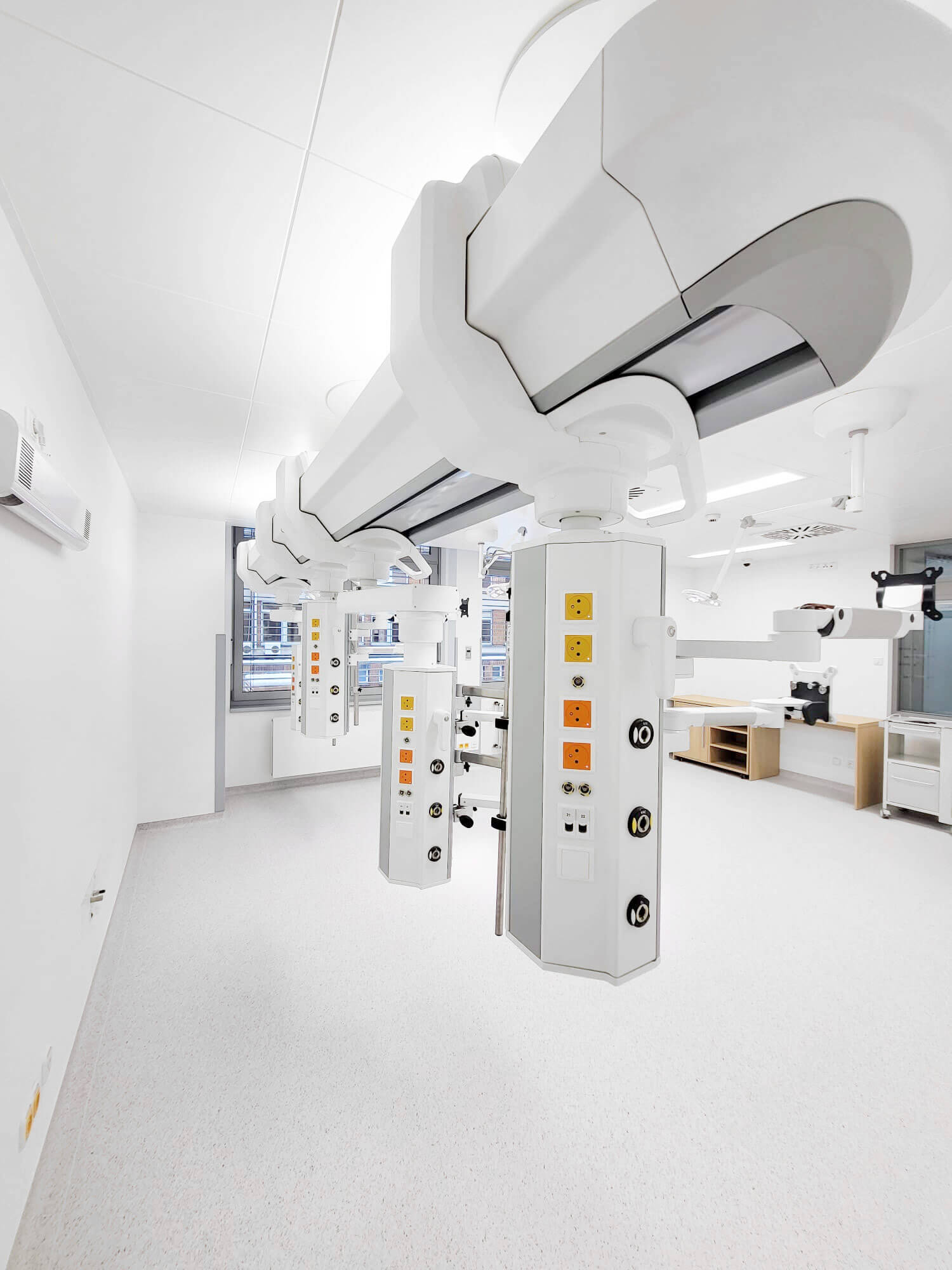
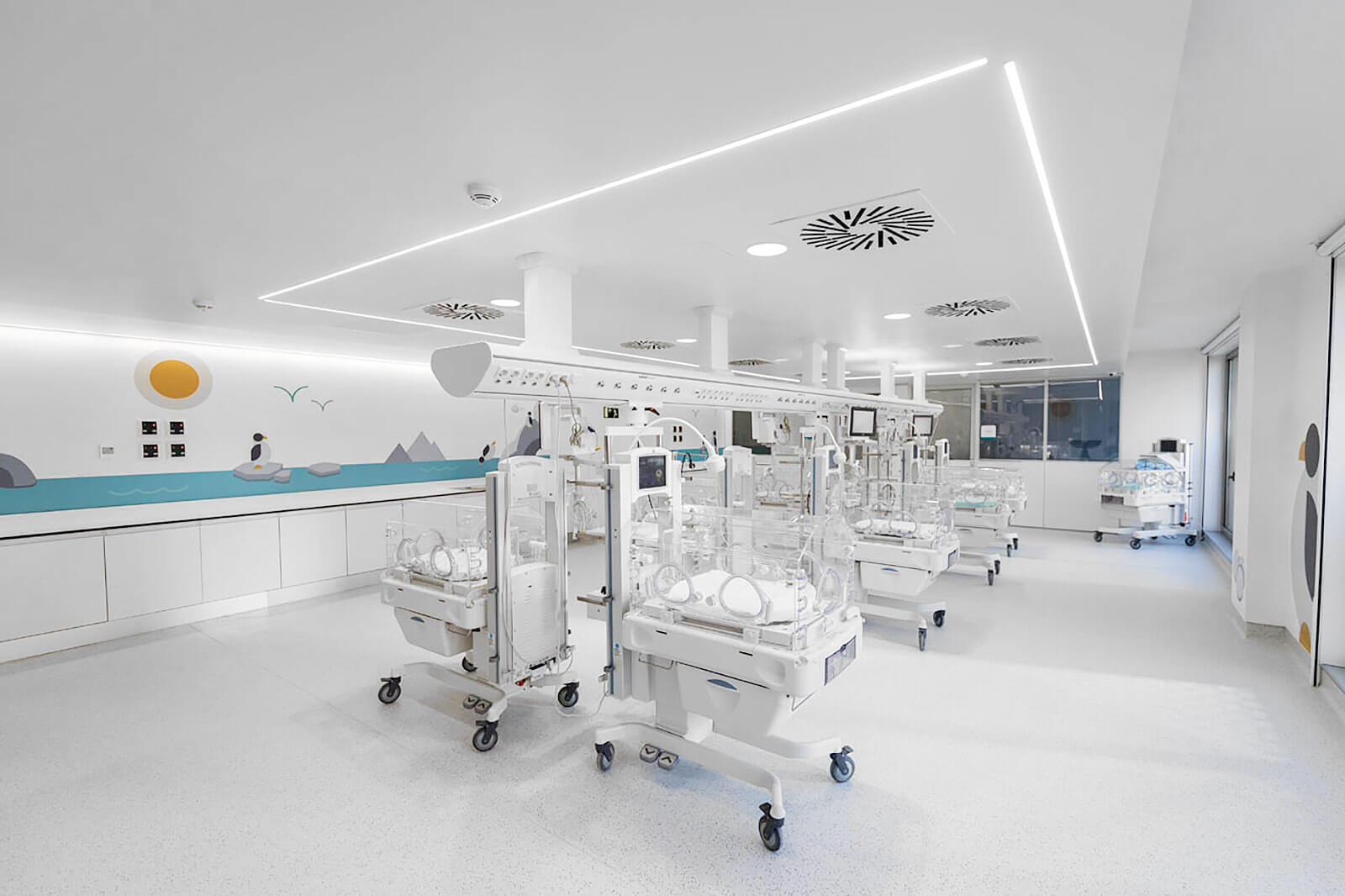
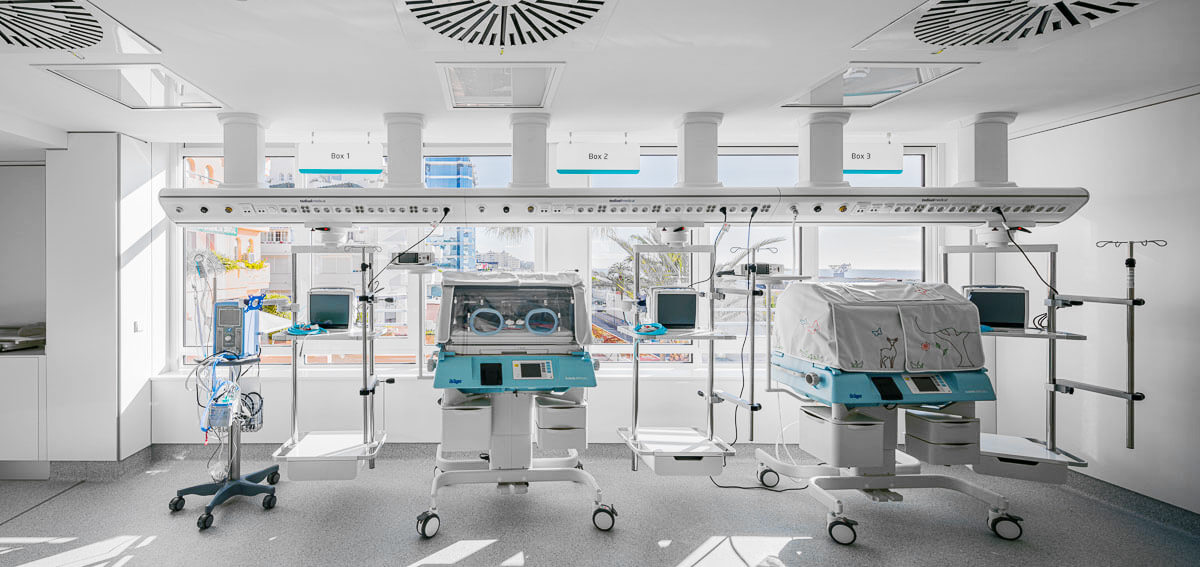
Optimizing workflow and safety in operating rooms, ICUs, and critical care wards to improve patient care
Hospitals and healthcare centers are currently facing one of the greatest challenges in their history: the constant increase in patients, the growing complexity of clinical procedures, and a shortage of healthcare personnel. This situation necessitates improved coordination, communication, and operational efficiency, especially in highly complex areas such as operating rooms, Intensive Care Units (ICUs), and critical care wards.
In this context, healthcare technology companies like Tediselmedical have developed advanced digital solutions based on the interconnection of devices, software, and hospital systems. These technological solutions allow for real-time patient flow management, resource optimization, and improved clinical safety, generating a direct impact on the quality of care.
This article analyzes in depth how digitization and intelligent workflow management are transforming the hospital environment, bringing tangible benefits to patients, healthcare professionals and organizations.
The importance of patient flow management in hospitals
Patient flow management is a strategic process that encompasses the coordination of people, resources, information, and time within the hospital. In critical areas, any delay or error can directly impact patient safety and clinical outcomes.
Among the main challenges are:
- Overburdened care
- Lack of real-time process visibility
- Frequent workflow interruptions
- Inefficiency in the use of resources
- Safety and hygiene risks
- Communication problems between teams
Digitization allows us to address these challenges through interconnected systems that provide real-time data and automated processes.
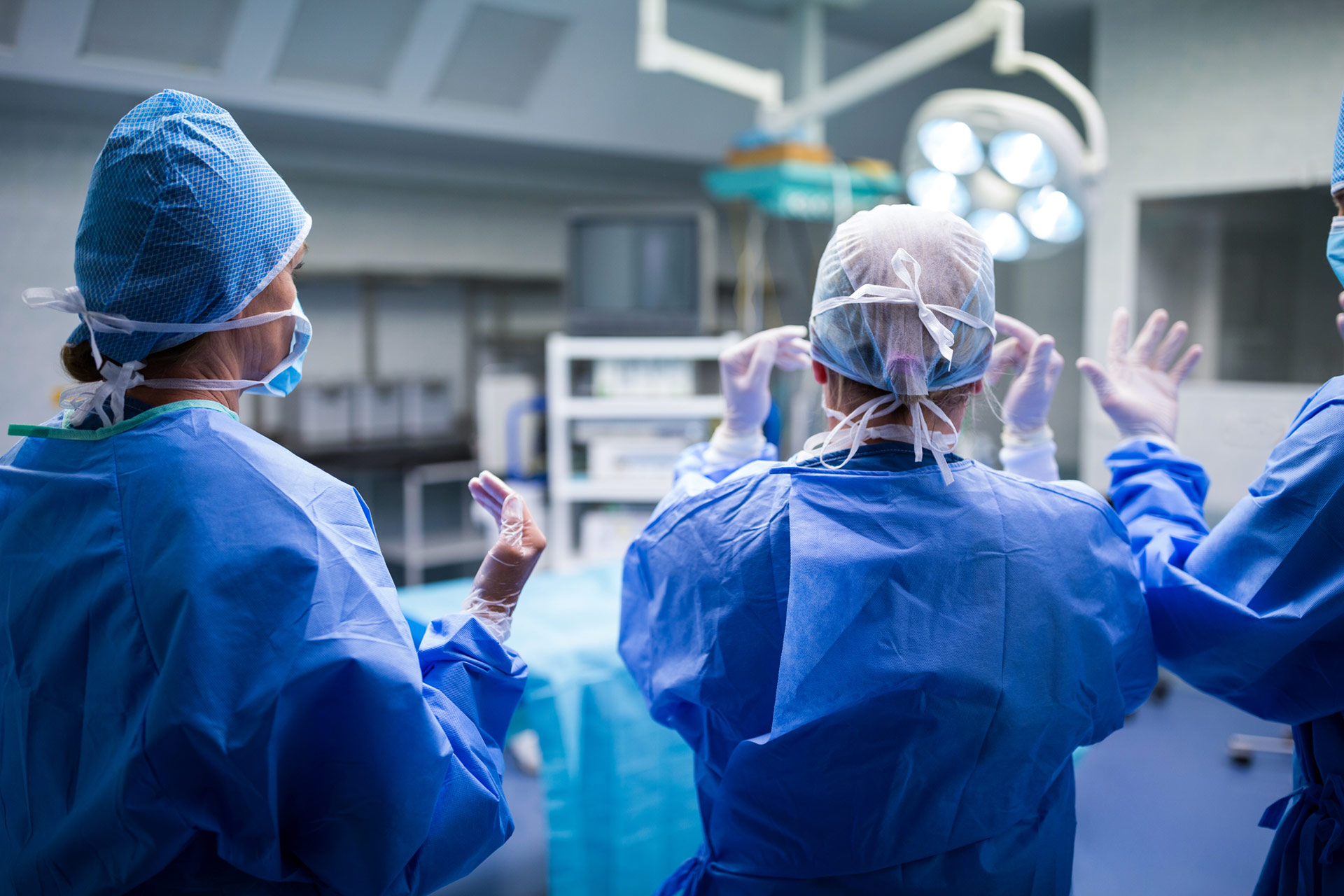
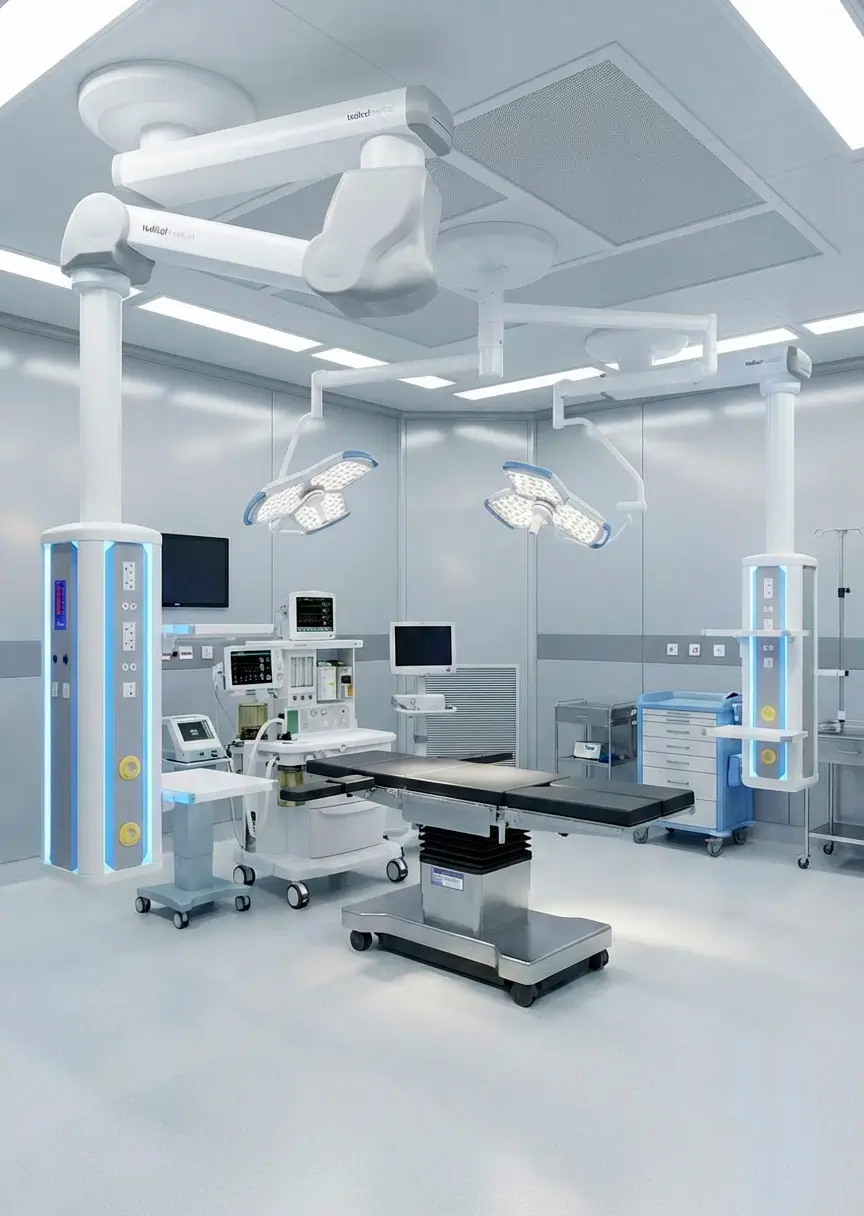
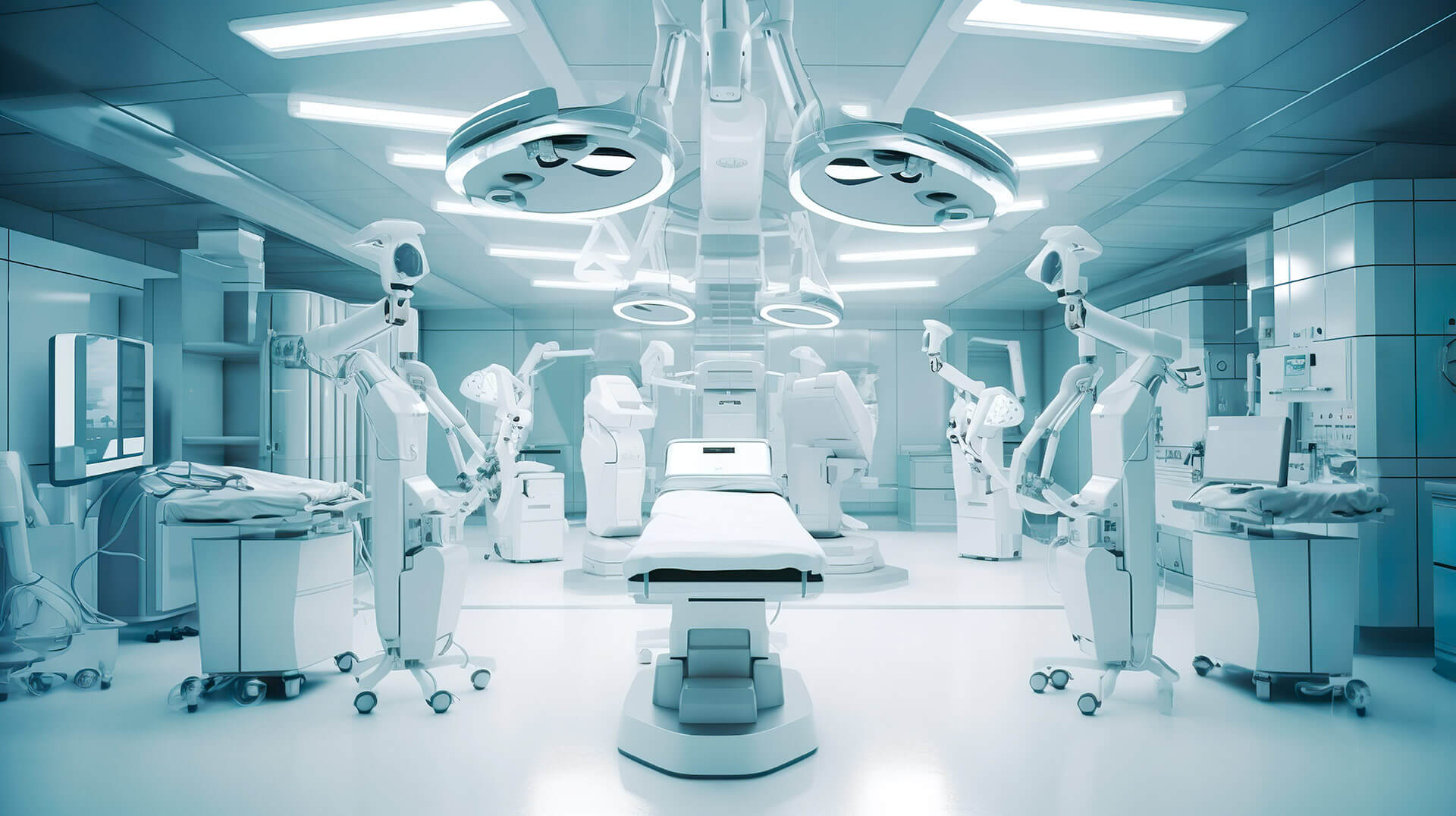
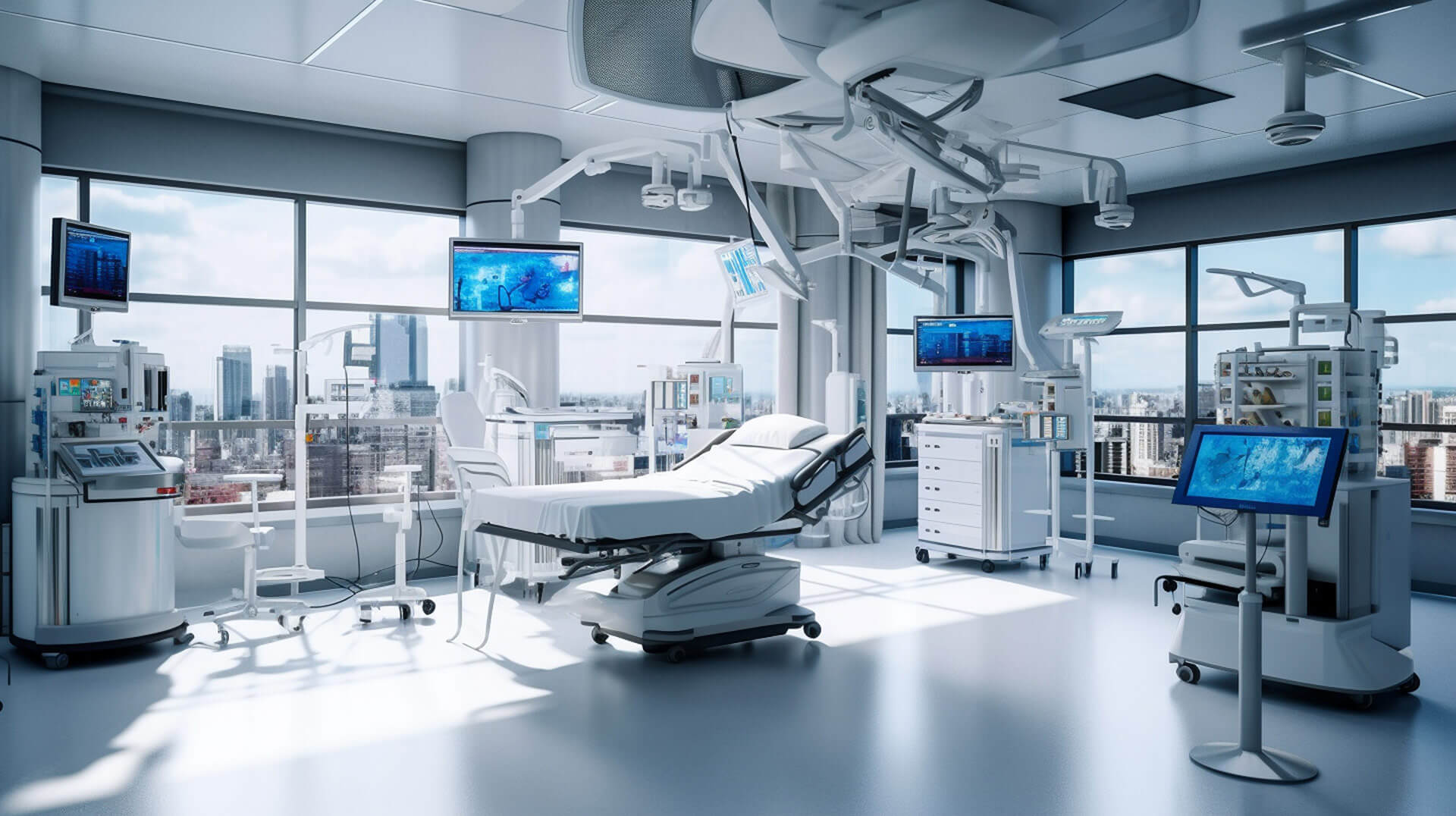
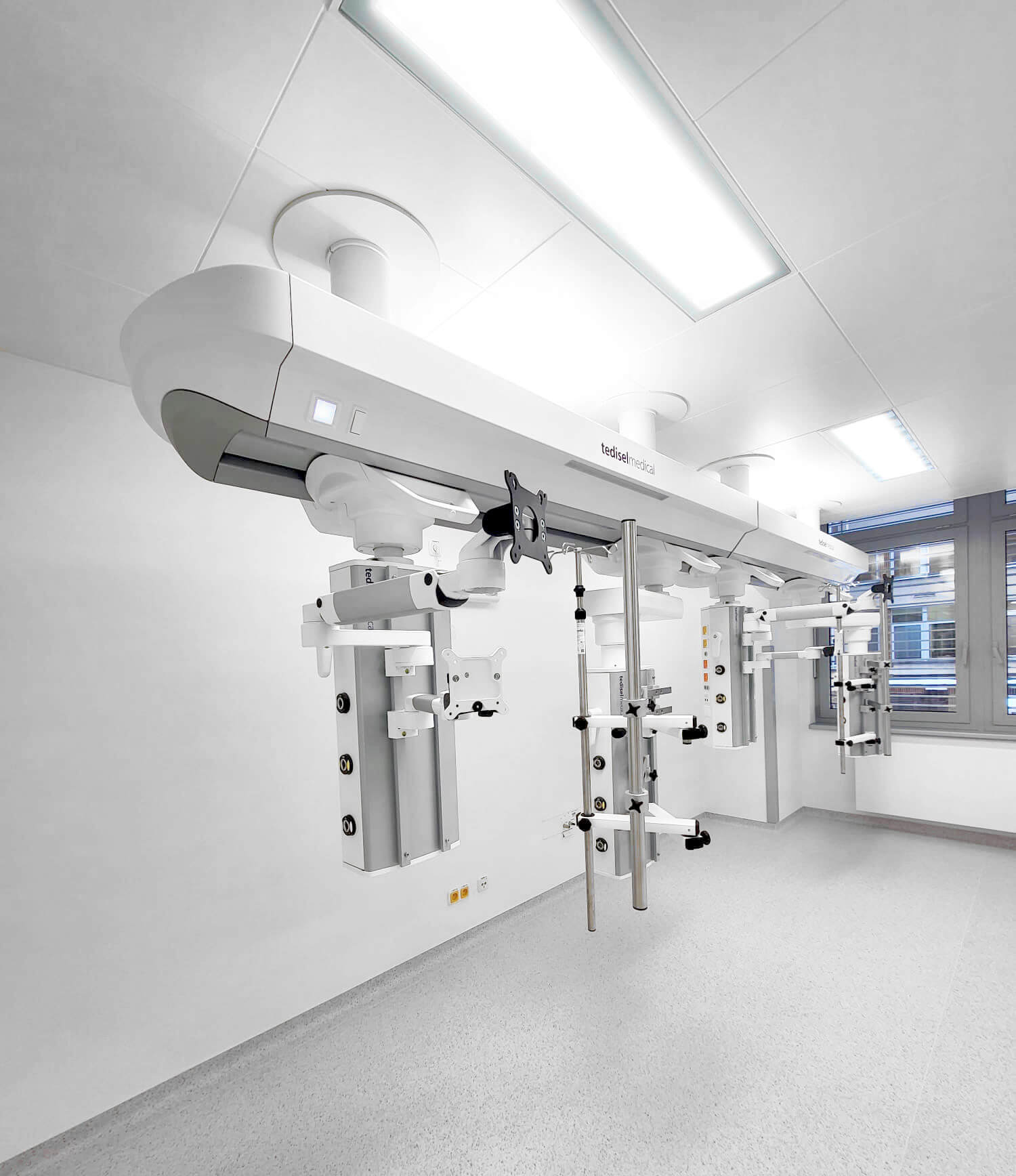
Digital ecosystems for operating rooms, ICUs and critical care wards
A digital hospital ecosystem consists of the integration of medical devices, technical infrastructure, and HERMES software on a single platform that connects information and operations.
This approach enables:
- Centralized control of equipment and resources
- Real-time communication between professionals
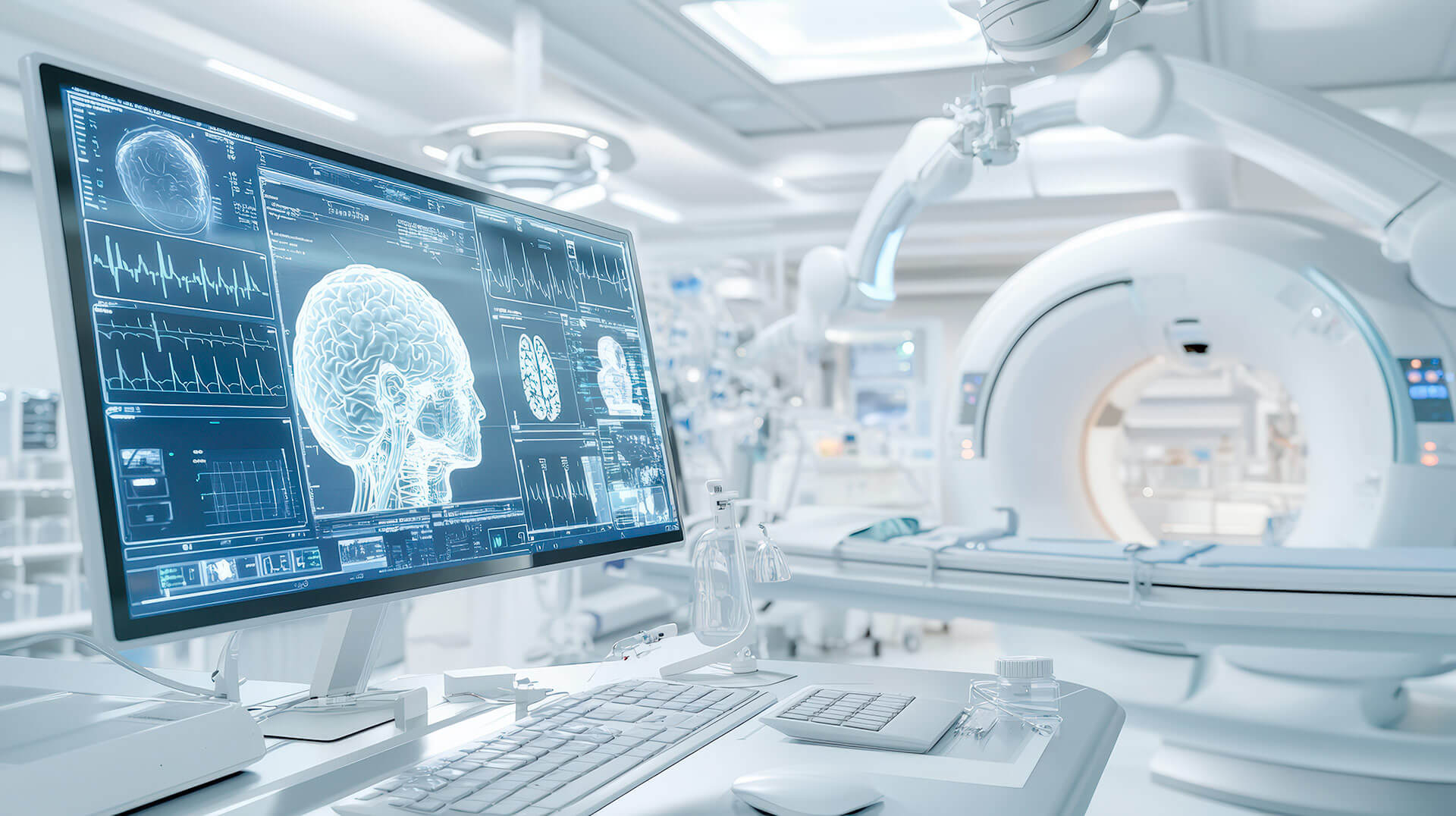
- Continuous monitoring of patients and processes
- Automation of operational tasks
- Improved clinical traceability
In operating rooms and ICUs, where precision and time are crucial, this integration reduces variability and improves the coordination of the healthcare team.
Horizontal and vertical interconnection
Interconnection is the key element that enables the efficient functioning of the digital ecosystem.
Horizontal Interconnection
Refers to the connection between patient-centered devices within the same room. Examples:
- Vital signs monitors
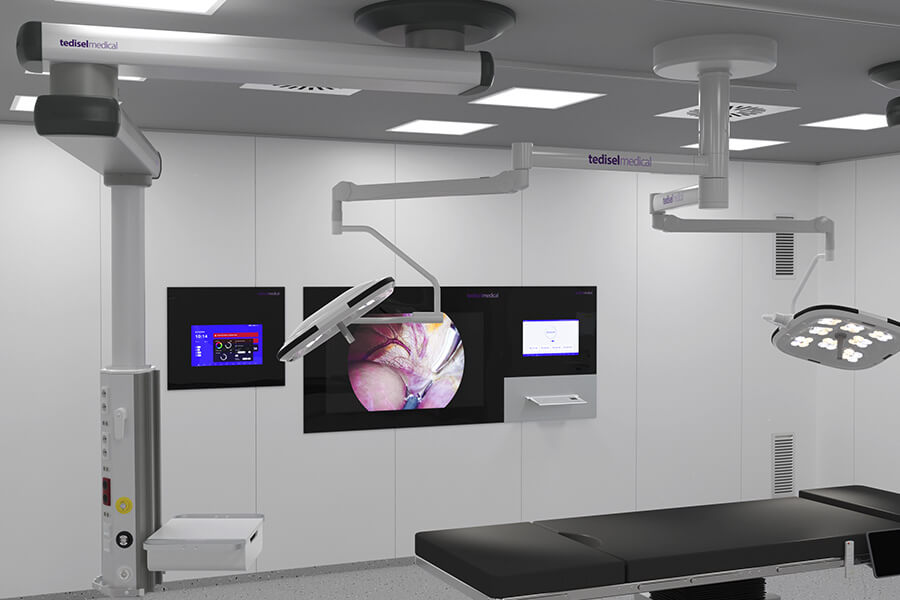
- Roof supply units
- Surgical lighting systems
- Anesthesia equipment
- Infusion Pumps
This integration facilitates immediate access to information and allows device synchronization
Vertical Interconnection
This refers to the connection between devices and hospital information systems. This enables:
- Automatic recording of clinical data
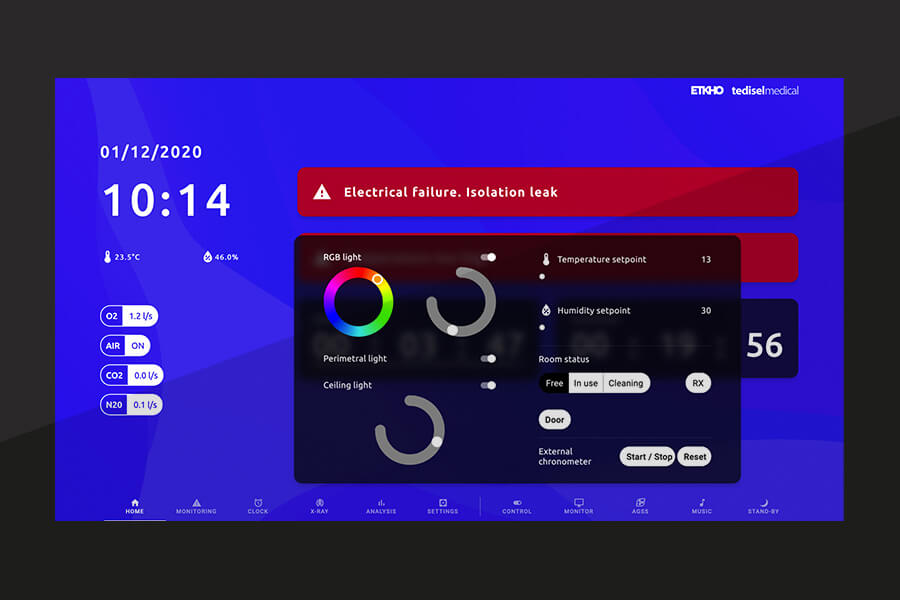
- Environmental control of the room (temperature, humidity, lighting)
- Alarm and notification management
- Integration with surgical planning
- Optimizing the use of resources
In a modern operating room, ceiling supply units can incorporate software that controls brakes, circadian lighting, and specific equipment functions, while integrating with the hospital’s information system to manage environmental and operational parameters.
Benefits of digital patient flow management
- Greater departmental efficiency
Automation and real-time visibility allow for reduced downtime and optimized surgical scheduling, improving hospital productivity. - Saving work time
Digital systems eliminate repetitive manual tasks, reducing unnecessary movement within the room and freeing up time for clinical care. - Error Reduction
Device integration and automatic data logging decrease human error, especially in critical environments where accuracy is essential - Workflow optimization
Standardized processes and centralized communication allow for improved coordination between multidisciplinary teams. - Greater safety and hygiene
Equipment traceability and procedure monitoring contribute to compliance with safety and infection control protocols. - Improved patient experience
Faster, more coordinated, and safer care directly impacts patient satisfaction and better clinical outcomes.
Impact on healthcare professionals
Digital transformation not only benefits the patient, but also the healthcare staff.
- Reduction of work-related stress
Automation and process visibility reduce uncertainty and the cognitive load on staff. - Improved communication
Integrated systems facilitate coordination between anesthesiologists, surgeons, nursing and technical staff. - Greater safety at work
Monitoring and centralized control allow for the detection of risks and rapid action. - Facilitating clinical work
Immediate access to relevant data improves decision-making and healthcare efficiency.

Impact on hospital management
From an organizational perspective, the digitization of the patient flow offers strategic advantages:
- Improved operational performance
- Optimizing the use of resources
- Reduction of operating costs
- Greater planning capacity
- Increased quality of care
- Improved security indicators
This positions the hospital in a competitive environment and prepared to meet future healthcare demands.
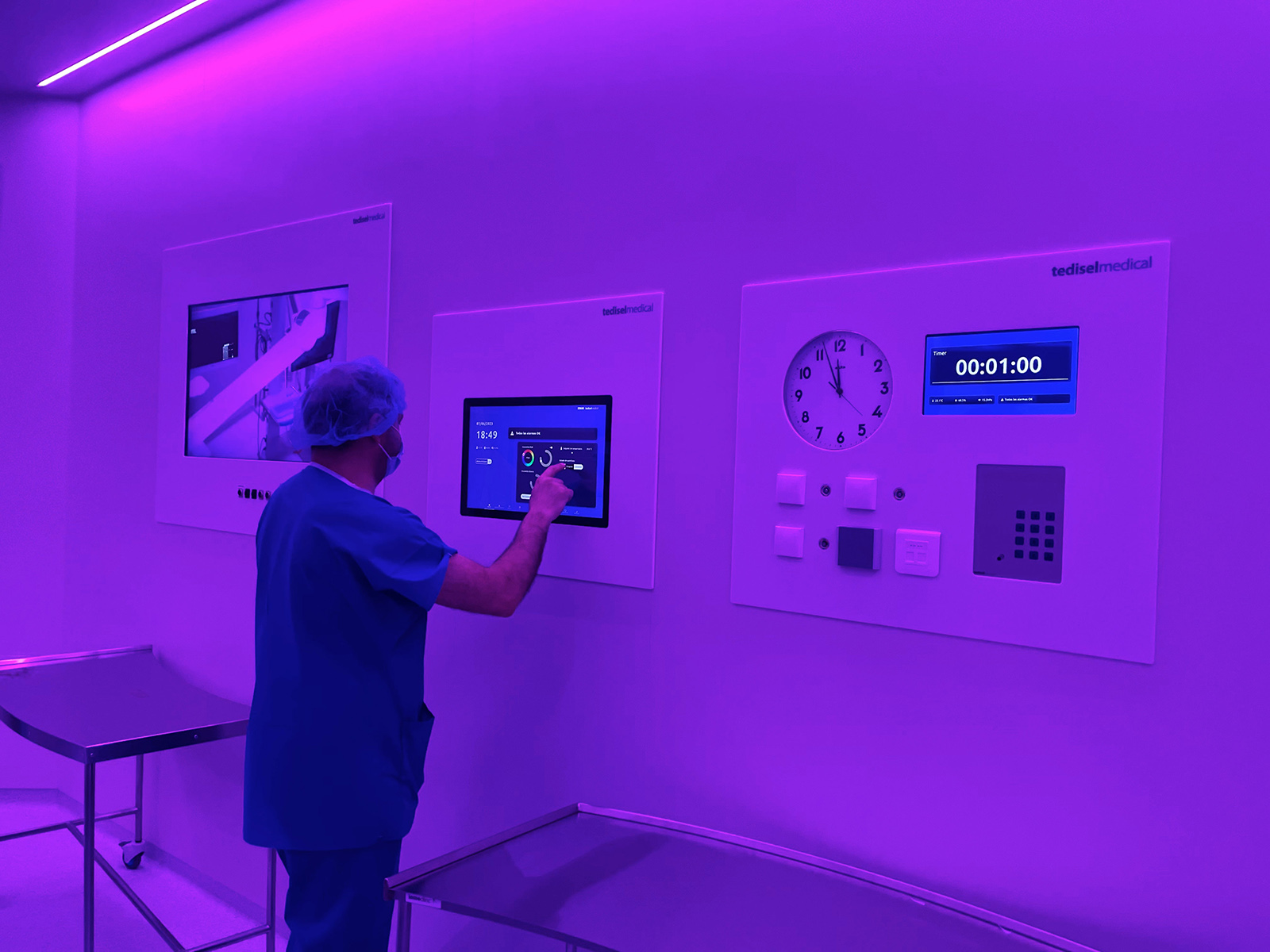
Intelligent environmental control in critical rooms
The physical environment of the operating room and the ICU is crucial for patient safety and the success of the procedure.
Digital systems allow control of:
- Temperature
- Humidity
- Differential Pressure
- Lighting
- Air Quality
This automated control improves infection prevention and the patient’s clinical stability
Reduction of disruptions in critical areas
Interruptions in the operating room or ICU can lead to errors and delays. Digital systems reduce these interruptions by:
- Automated notifications
- Real-time information panels
- Centralized communication
- Automation of resource requests
- Integration with hospital logistics
This promotes continuity of workflow and patient safety.
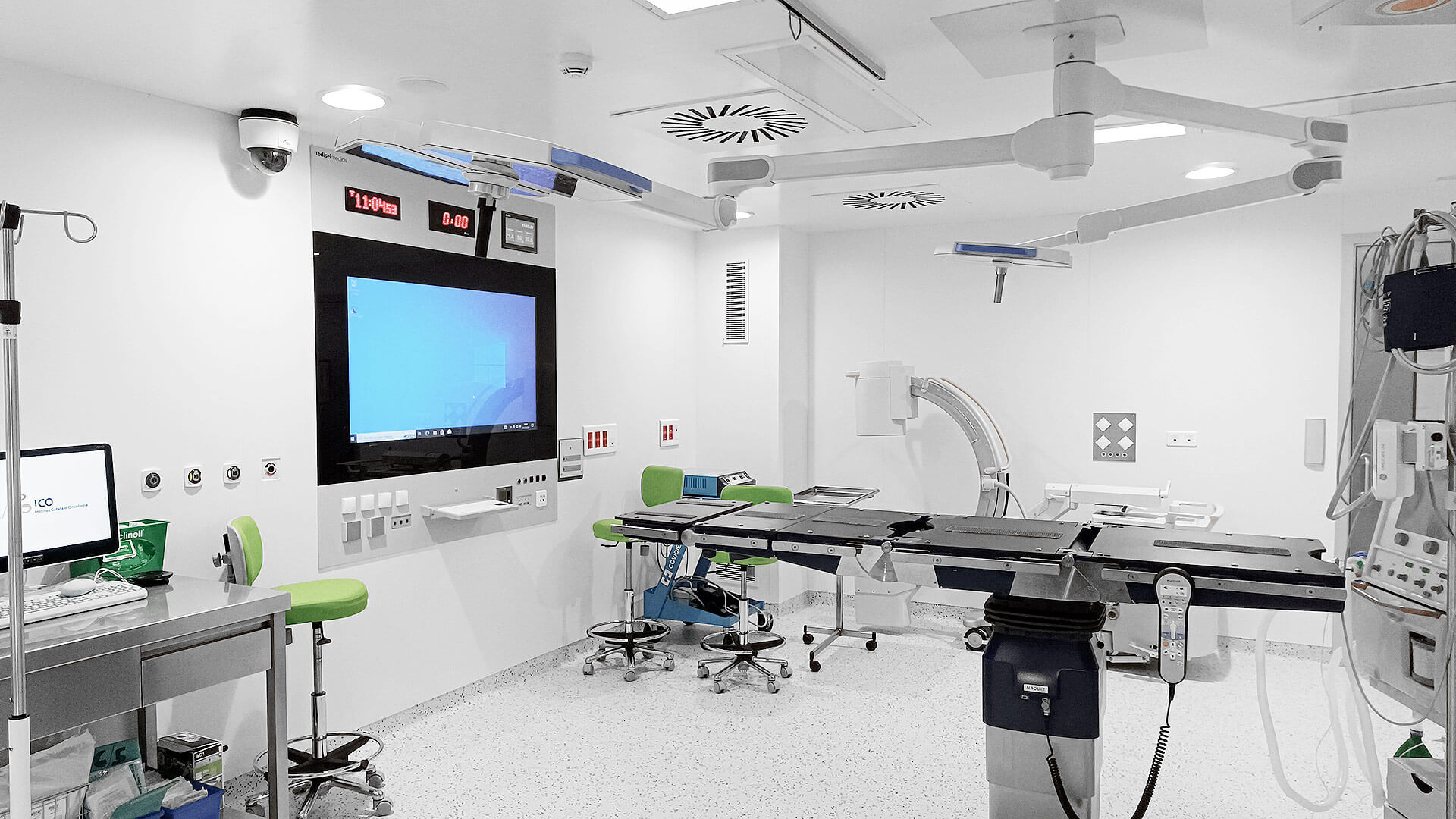
Transforming the operating room into the smart operating room
The concept of a smart operating room integrates technology, connectivity, and automation to create a highly efficient environment.
Key Features:
- Full integration of medical devices
- Centralized room control
- Automatic data recording
- Environmental monitoring
- Advanced audiovisual communication
- Decision support
This model improves surgical precision, reduces time, and optimizes the clinical team’s experience.
Importance of simple and scalable integration
One of the critical factors for technology adoption is the ease of integration with existing infrastructures.
Modern solutions should offer:
- Compatibility with hospital systems
- Scalable architecture
- Customization to meet needs
- Data security
- Continuous updates
- Interoperability between devices
Integration capabilities ensure a lasting and sustainable impact on healthcare
Future of patient flow management
Technological evolution will continue to transform the hospital environment through:
- Artificial intelligence applied to surgical planning
- Predictive analytics of patient flow
- Hospital Logistics Automation
- Advanced Remote Monitoring
These innovations will enable more efficient, safer, and patient-centered hospitals.
Optimizing workflow and safety in operating rooms, ICUs, and critical care units is a strategic priority for modern hospitals. Implementing interconnected digital ecosystems improves coordination, reduces errors, and increases operational efficiency.
The horizontal and vertical integration of devices, along with intelligent environmental control and process automation, transforms the clinical environment into a safer and more efficient system. This change benefits not only the patient, but also healthcare staff and hospital management.
Digitizing patient flow is no longer an option, but a necessity to meet the current challenges of the healthcare sector and ensure high-quality care in critical environments.